Implants and bone augmentation
Received: 04-May-2020, Manuscript No. PULDCR-20-10248; Editor assigned: 07-May-2020, Pre QC No. PULDCR-20-10248 (QC); Reviewed: 21-May-2020 QC No. PULDCR-20-10248; Revised: 22-Jul-2022, Manuscript No. PULDCR-20-10248 (R); Published: 19-Aug-2022
Citation: Malefakis Manolis. Implants and bone augmentation. Dent Case Rep 2022;6(4):1-3.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
The use of endosseous implants provides dentistry, the solution in many problems. Someone who worked in early 90's may remember, the full arch reconstructions in periodontal teeth, the heroic attempts for endodontic treatments, root-end resections (palatal roots of molars, mandibular premolars), root resections/root separations of molars. Today no uses these approaches, because our patients after spending time, effort, and money, want solutions with proven durability, solutions that only endosseous implants can provide. In fixed prostodontics, natural bone, late loading, good surgery, the failure rate is something like 2%. A study comprising of 4641 branemark dental implants for a period of 3 years and reported a failure rate of 1.5%.
Keywords
Dentistry; Palatal roots; Periodontal teeth; Patients
Introduction
Bone expansion for dental inserts is once in a while important when a patient needs more bone accessible to secure the screw or other embeds equipment appropriately. Dental bone increase incorporates different methods, including sinus lifts, bone unite strategies, and control of bone utilizing an osteotome or osteotome hammer [1]. Since an embed isn't possible without a specific measure of bone accessible, it becomes fundamental for a periodontal specialist to animate the patient to develop more bone nearby, or to eliminate bone from one region and spot it in the space where the embed will be finished.
Bone expansion methodology in embed dentistry are normal, particularly in instances of bone decay, where tooth misfortune without substitution has caused the disintegration of bone after some time [2-6]. Bone increase a medical procedure should be possible to work on the probability of having the option to put an embed; however it requires embed a medical procedure to be postponed while the bone mends
The use of endosseous implants provides dentistry, the solution in many problems. Someone who worked in early 90's may remember, the full arch reconstructions in periodontal teeth, the heroic attempts for endodontic treatments, root-end resections (palatal roots of molars, mandibular premolars), root resections/root separations of molars. Today no uses these approaches, because our patients after spending time, effort, and money, want solutions with proven durability, solutions that only endosseous implants can provide. In fixed prostodontics, natural bone, late loading, good surgery, the failure rate is something like 2%. A study comprising of 4641 branemark dental implants for a period of 3 years and reported a failure rate of 1.5%. My statistics in these conditions are 1%. Failure rate in immediate loading rise (9%), also in maxillary over dentures with 4 implants freestanding (15%), and when I use implants to salvage removable partial dentures (20%). It is believed that in the field of general dentistry the failure rate is bigger [7-12]. Also when we use removable interim rehabilitations we have to expect high failure rates. I had a patient with a removable interim rehabilitation, and he gave me in the hand the implant after one week, (was inserted with torque 55 Ncm and closed with the gingiva).
Case Presentation
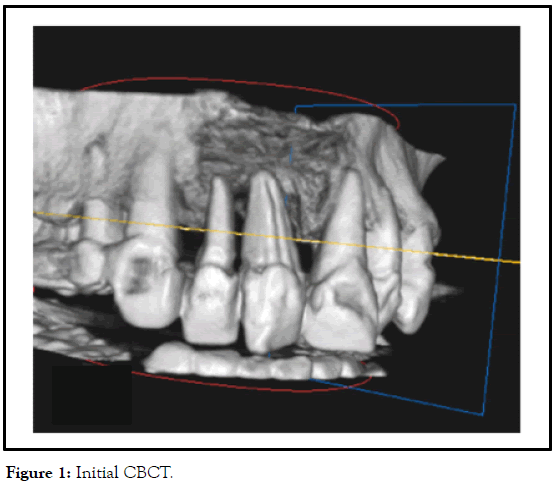
The replacement of two periodontal involved teeth (right central and lateral incisors/maxilla). Gingival crevices measured more than 10 mm, and the intraoral X-ray revealed complete absence of bone. CBCT affirmed the absence of alveolar bone, but revealed bone 4 mm-5 mm under the nose, and the disappointing periodontal condition of left central incisor (Figure 1).
The patient insisted in the replacement of the incisors with the use of dental implants. In the conversation about bone reconstruction of the area, I told her, that the possibilities of reconstruction with guided bone regeneration were few. The use of a fixed bridge was more difficult, because I had to extract and the left central incisor, and use as abutments, at least right canine, left lateral incisor and left canine, and having a bridge with tree pontics. Three pontic prosthesis flexes 18 times more than two pontic prosthesis, whereas a two-pontic restoration flexes eight times more than one-pontic prosthesis.
Results and Discussion
We agree to use as graft, cerabone (natural bovine bone graft) as steak bone with PRF/platelet rich fibrin, with membrane cytoplast Ti-250 XL (d-PTFE, reinforced with Ti), and as provisional, a Maryland bridge. Teeth of Maryland were from acrylic in order to change them easily. I did the extractions the same day (I had already the provisional) the patient received table Augmentin 625 mgr/8 h two days before and 6 days after, topical anesthesia articain 1/100.000. The blood collected from me, and PRF used in small pieces with the graft, and as a membrane under the d-PTFE membrane. Maryland was used with adhesive resin without the use of primer AMD adhesive liquids, in order to remove it easily. Except antibiotics, patient is given PRUFEN 400 mgr/6 days and chlorfexidine mouyhwash 0.2%, twice per day for two weeks (Figure 2).
The result, (the flap is stretched too much, the vascularization was compromised and there was dehiscence, that is the reason for using d-PTFE membrane). In order to avoid dehiscence, we should have waited three months for the healing of the soft tissues. [Complex three-dimensional bony defects command large volumes of bony augmentation that require tensionfree soft-tissue closure to maintain blood supply to the grafted area [13]. This also prevents incision line opening, the number one complication of large alveolar bone grafts. Preliminary soft-tissue augmentation utilizes both allogeneic tissue (freeze-dried human dermis), as well as autogenous tissue (palatal connective tissue), to prevent vestibular dehiscence, another common complication following alveolar bone grafts. Three months of healing is required prior to bone grafting.
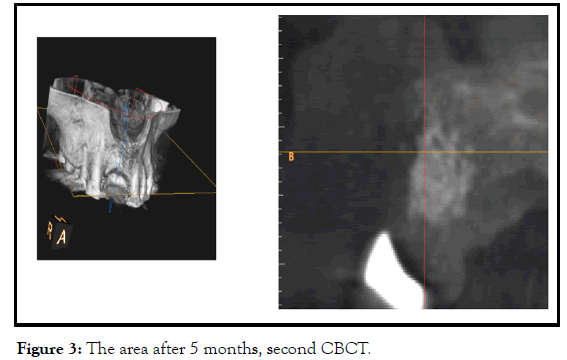
After five months, radiographically, was enough osseous regeneration. In opening to install the implants, portion of the graft was not resorbed, but because of the haemorrhage from the graft, I thought that was integrated, and there was no need for further waiting. osseointegration of the implant does not occur until the grafted bone has become vascularized (Figure 3).
Two implants have been used, Alpha-Bio Neo/3.2 mm, and 13 mm in length (topical anesthesia articain 1/100.000). Reasons for using this implant were one. Primary stability, in the native bone, because of the aggressive threads. Small diameter, possibly I need only the pilot drill. I used piezoelectric surgery for the preparation of the implants wells, in order to avoid vibrations, common with the use of micromotor. As surgical guide, we used a clear copy of the Maryland [14].
The problem was the slight mobility of the graft and the fact that the implants installed with screwing and were taking the final position not coincident with the implant osteotomy, so the distance between them, was slight less than 3 mm.
Some implants, such as those with an aggressive thread design, may change the drilling path and angulation, and this three-dimensional change commonly occurs as the implant is being torqued in place; the implant is following the path of least resistance within the alveolus.
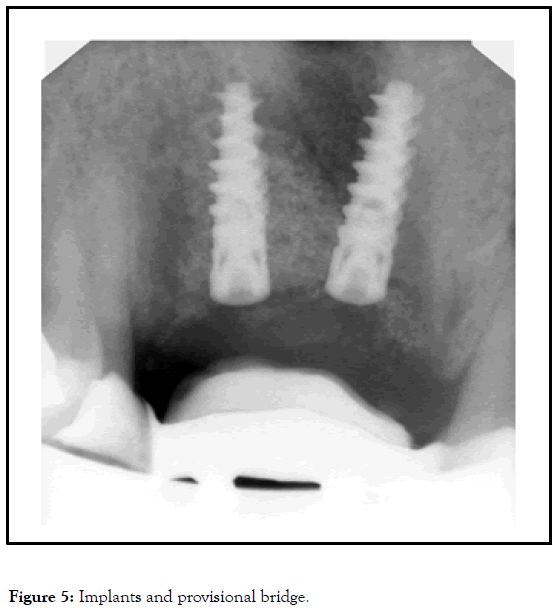
Implant Aesthetics, Keys to Diagnosis and Treatment. The final torque was 40 N*cm, and I had the fear to lose the graft; implants remain in that position (Figures 4 and 5).
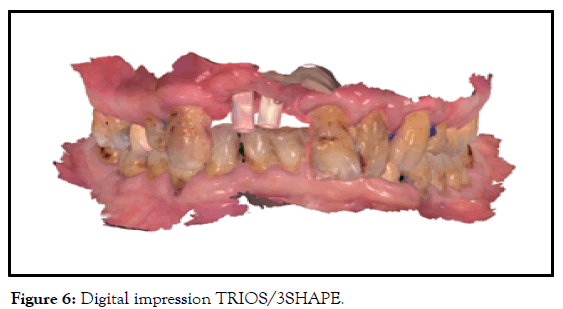
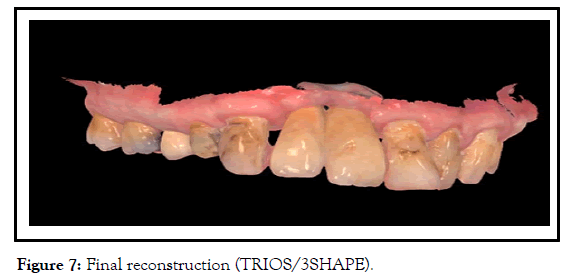
Final reconstruction installed in August 2019 was, splinted/screwed/ zirconium crowns, with Ti bases (Figures 6 and 7).
Because when smiling, the upper lip ascends to the middle of central incisors, the aeshetics were acceptable, and this was one reason for not using provisionals and the other was to have the definite restoration earlier [15-17].
Conclusion
Simple or medium scale cases, with implants-guided bone regenerationprosthodontics with the use of new instruments, techniques and materials intraoral scanner, piezosurgery, d-PTFE membranes, PRF is possible to achieve, in the area of a typical dental clinic.
REFERENCES
- Αdell R, Lekholm U, Rockler B, et al. A 15-year study of osseo integrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981;10:387-416.
[Crossref] [Google Scholar] [Pubmed]
- Friberg B, Jemt T, Lekholm U. Early failures in 4,641 consecutively placed Brånemark dental implants: A study from stage 1 surgery to the connection of completed prostheses. Int J Oral Maxillofac Implants. 1991;6(2):142-6.
[Google Scholar] [Pubmed]
- Rasoul HP, Mina KA, Ali M. Risk factors and early survival rate of biomet 3I dental implants: A retrospective study. J Dentomaxillofacial Radiol Pathol Surg. 2015;4(1).
- Matthew PH, Jaffer A, Shariff DDS, et al. Incidence and determinants of dental implant failure: A review of electronic health records in a U.S. dental school. J Dent Educ. 2016;81(10):1233-42.
[Crossref] [Google Scholar] [Pubmed]
- John D, Da Silva, Julie K, et al. Outcomes of implants and restorations placed in general dental practices for the practitioners engaged in applied research and learning network group. 2014;704-13.
[Crossref] [Google Scholar] [Pubmed]
- Cristina P, Laura M, David P, et al. Risk factors associated with early failure of dental implants. A literature review. Med Oral Patol Oral Cir Bucal. 2011;16(4):514-7.
[Crossref] [Google Scholar] [Pubmed]
- Mohammad J, Mohammad B, Amir H, et al. Analysis of the factors affecting surgical success of implants placed in iranian warfare victims. Med Princ Pract. 2016;25:449-54.
[Crossref] [Google Scholar] [Pubmed]
- Bandeira de Almeida A, Prado Maia L, Ramos UD, et al. Success, survival and failure rates of dental implants: A cross-sectional study. J Oral Sci Rehabilit. 2017;3(1):24–31.
- Bashutski JD, D'Silva NJ, Wang HL. Implant compression necrosis: Current understanding and case report. J Periodontol 2009;80:700-4.
[Crossref] [Google Scholar] [Pubmed]
- Bidra A, Daubert D, Garcia L, et al. Clinical practice guidelines for recall and maintenance of patients with tooth-borne and implant-borne dental restoration. J Prosthodont 2015;25:S32–S40.
[Crossref] [Google Scholar] [Pubmed]
- Brunski JB. In vivo bone response to biomechanical loading at the bone/dental implant Interface. Adv Dent Res. 1999;13:99-119.
[Crossref] [Google Scholar] [Pubmed]
- Esposito M, Hirsch JM, Lekholm U, et al. Biological factors contributing to failures of osseointegrated oral implants. I. Success criteria and epidemiology. Eur J Oral Sci. 1998;106:527-551.
[Crossref] [Google Scholar] [Pubmed]
- Flemmig TF, Beikler T. Decision making in implant dentistry: An evidence based and decision-analysis approach. Periodontol. 2009;50:154-72.
[Crossref] [Google Scholar] [Pubmed]
- Furst MM, Salvi GE, Lang NP, et al. Bacterial colonization immediately after installation on oral titanium implants. Clin Oral Implants Res. 2007;18:501-8.
[Crossref] [Google Scholar] [Pubmed]
- Heitz-Mayfield LJ. Peri implant diseases: Diagnosis and risk indicators. J Clin Periodontol. 2008;35:292-304.
[Crossref] [Google Scholar] [Pubmed]
- Koldsland OC, Scheie AA, Aass AM. The association between selected risk indicators and severity of peri-implantitis using mixed model analyses. J Clin Periodontol. 2011;38:285-92.
[Crossref] [Google Scholar] [Pubmed]
- Lang NP, Wilson TG, Corbet EF. Biological complications with dental implants: Their prevention, diagnosis and treatment. Clinical Oral Implants Res. 2000;11:146-55.
[Crossref] [Google Scholar] [Pubmed]