Medical specialist’s perceptions and expectations of subspecialist training in the developing world
Received: 01-Aug-2017 Accepted Date: Aug 08, 2017; Published: 15-Aug-2017
Citation: Dalmeyer JPF, Sruwig M. Medical specialist’s perceptions and expectations of subspecialist training in the developing world. J Reprod Biol Endocrinol. 2017;1(1):1-2.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
The shortage of healthcare workers and doctors in the developing world compared to the developed world is a problem due to the continual migration of qualified professionals and the inability of the state to remedy these shortfalls [1]. The private hospital groups in South Africa and other private corporates have over the last number of years taken limited initiative to fund education projects in conjunction with the academic institutions. However, these projects have been poorly focused and have been managed in an unstructured and detached manner. There is hence a desire from the private sector to get involved in these projects on a much larger scale through more formalised structures [2].
In South Africa, higher education has reached a turning point. Medical education, in particular, needs to adapt to accommodate the changes of subspecialty training and education. South Africa needs to increase the numbers and the quality of higher-educated clinicians, to serve this fastdeveloping country [3].
A trial model for training subspecialists in reproductive medicine was developed as a pilot project to address the threatening shortages and training duration [4]. To further investigate what needs to be done regarding the training of subspecialist, the perceptions and expectations of subspecialists [reproductive subspecialists and cardiologists] regarding subspecialty training were collected. This editorial on is a brief overview of the research. To conclude recommendations are provided.
Background and A Brief Overview of The Study
Since South Africa’s transition to democracy in 1994, inequality in South African society is still the main obstacle to economic growth. Unemployment thus far has been the single largest barrier to realising economic growth, and it will be so for a long time to come [5].
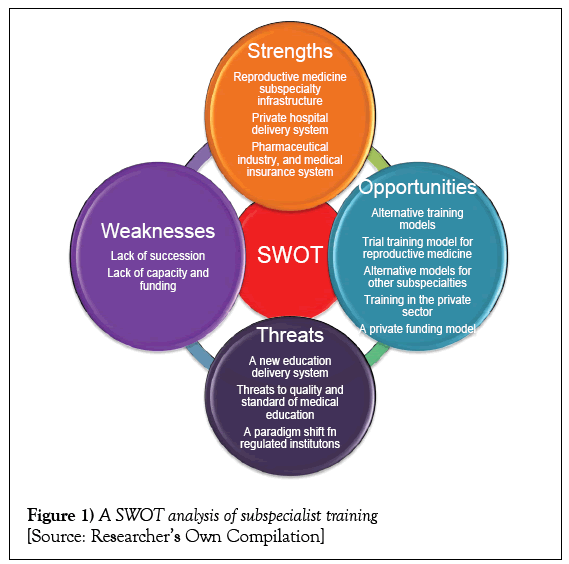
A SWOT analysis is one of many possible strategic planning tools used to evaluate the strengths, weaknesses, opportunities, and threats involved in a project, or any other situation requiring a decision [6]. This general business analysis method is applied to understand the environment in which medical subspecialty training take place. A graphic overview of the SWOT analysis of the training environment of medical subspecialists is provided in Figure 1.
It is further clear from the literature that the length of training required to reach the level of subspecialty fellow is a concern in the training programmes for subspecialists [7].
The Empirical Study and Results
To investigate Medical specialists’ perceptions and expectations of subspecialist training in the developing world 214 gynaecologists were requested to complete online questionnaire. Cardiologists were requested via their newsletter to complete the online questionnaire. Of the 214 emails that were sent, 66 responses were received from the reproductive medicine subspecialists. Fourteen cardiologists responded to the newsletter invitation that was sent. The total number of respondents was thus 80 and was an adequate number for an exploratory study.
The majority of the respondents was males, in the age group of 55-59 years and had practising experience of more than 10 years. The overall results show that there was the intention among respondents to expand their practices. This finding applies particularly in the case of the reproductive medicine respondents. The majority of the respondents were practising close to academic institutions and major private hospitals. The results indicate that the cardiology respondents tended to conduct their practice as solo practitioners, while the reproductive medicine respondents tended to operate in group practice.
The results of the demographic variables confirm the aging profile of subspecialist and the need to ensure succession. The results further showed that cardiologists and reproductive subspecialist expectations of the training of subspecialists are very similar except for their expectations on the training duration. Reproductive subspecialist respondents agreed more than cardiology subspecialist respondents that the training duration is too long. The biggest gap between perceptions and expectations is also with the factor training. The results showed that the expectations of subspecialists are not met for training.
Only six variables were met for the cardiologists, while only three variables were met for the reproductive medicine specialists. The three areas where reproductive specialist seems to be satisfied include:
•Supernumerary reduces training capacity
•PPP will contribute to a successful NHI
•SASREG accredited subspecialists are in practice
The areas, which require attention, where expectations have not been met, according to the cardiologists, are the following:
Dalmeyer et al
•That the number of subspecialists is adequate,
•That the particular subspecialist training programme serves demand,
•That current training infrastructure is acceptable,
•That current training capacity is adequate,
•That current training capacity is acceptable,
•That current public-sector infrastructure is acceptable,
•That academic institutions have adequate training capacity,
•That practising a subspecialty without having completed a fellowship is acceptable, and
•That public/state training facilities offer adequate training opportunities.
•The areas which require attention, where expectations have not been met, according to the reproductive subspecialists, are:
•That current public-sector infrastructure is acceptable, and
•That current public-sector infrastructure is adequate.
Stakeholders in the medical profession at all levels have become aware of the looming crisis in terms of both service delivery and the sustaining of medical excellence. Our study confirmed that the training expectations of the respondents were not met.
Government’s current focus on primary health care creates additional challenges for specialist and subspecialist training. Over the years, the private sector has shown its willingness to invest in tertiary education. Unfortunately, though the funding has been done in a haphazard, uncoordinated way, and with vested interests.
The National Health Insurance [8] policy has highlighted the enormous shortage of healthcare workers at all levels over the next number of years. A successful model to train medical subspecialist are needed as it would contribute to addressing a substantial part of this shortfall, not only in terms of numbers of specialists, but also in maintaining the quality of medical education which South Africa has always been known for, both in the public and the private sector.
REFERENCES
- Naicker S, Ruhle PJ. Shortage of healthcare workers in developing countries. Ethn Dis. 2011;19:60-4.
- Discovery Foundation. Investing in medical education. Creating a healthier South Africa. The Discovery Foundation Awards 2012. Johannesburg. 2012.
- Buchen IH. The future of higher education and professional training. Foresight. 2005;7:4:13-21.
- Kruger TF. Statistical information obtained from the “Trial Project” on fellowship certification completions. Personal correspondence from the Faculty of Health Sciences, University of Stellenbosch. 2002-2012.
- Nel PS, Werner A, Poisat P, et al. Human resources management, 8th edition. Oxford University Press Southern Africa. Cape Town. 2011.
- Hellriegel D, Jackson SE, Slocum J, et al. Management. 4th ed. Cape Town: Oxford University Press. 2012.
- Freed G, Dunham K, Switalski K, et al. Pediatric fellows: perspectives on training and future scope of practice. Pediatrics – supplement article. 2009;31-7.
- NHI National Health Insurance for South Africa. Towards universal health coverage. Pretoria: Department of Health. 2003.