A case of Bowen disease arising in seborrheic keratosis
2 Department of Surgery, Shanghai Dermatology Hospital, Shanghai, China
3 Department of Pathematology, Shanghai Dermatology Hospital, Shanghai, China, Email: chenjia_doc@163.com
Received: 23-Jul-2018 Accepted Date: Aug 08, 2018; Published: 15-Aug-2018
Citation: Tan J, Chen X, Liu X, et al. A case of Bowen disease arising in seborrheic keratosis. J Dermatopathol. 2018;1(1):8-9.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Seborrheic Keratosis (SK) is one of the most benign epidermal neoplasms that rarely transform malignant. In this case, we report a SK malignant transformation to Bowen Disease (BD) with no relation to sun expose in China. The patient is a 72-year-old woman with a black skin lesion on her back. Clinical diagnosis of SK was made then a completely excision was performed. Histologically result showed a part of atypia keratinocytes with full-thickness in epidermis but no invasion to dermis arising in typical SK area. Thus, a pathologic diagnosis of BD arising in SK was made. This indicate that malignant transformation in SK can occur in the absence of sun expose.
Keywords
Seborrheic keratosis; Bowen disease; Malignant transformation
Introduction
Seborrheic keratosis (SK) is one of the most benign epidermal neoplasms that occurs in middle-aged or elderly people [1]. It is appearing more frequently in sun-exposed areas and can be easily found on face, trunk or extremities. The diagnosis is usually easy to made for the typical presenting as light or dark brown sharply demarcated plaques, papules, or patches stuck on the skin [2]. Though rare, reports of SK malignant transformation are increasing gradually. From recent retrospective study, the rate of SK malignant transformation is varying from 0.0006% to 7%. In which, the basal cell carcinoma (BCC) and Bowen’s disease (BD) are more frequent malignant type associate with SK [3,4]. Though the reasons of differences in malignant results are still no conclusion, BD arising from SK might associate with high solar UV radiation levels or HPV infection [4,5]. Here, we report a case of BD that arising within SK in the absence of sun expose in China.
Case Report
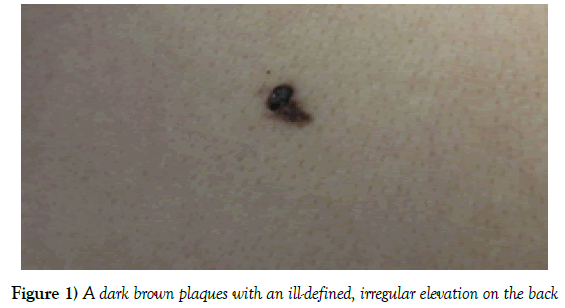
A 72-year-old woman consulted to our hospital due to a black skin lesion on her back with no other unusual symptoms. It had been present for decades but recently increased in size. The lesion was no infiltration observed and caused no subjective discomfort. The patient had no skin cancer family history. Physical examination revealed a 1 × 0.5 × 0.3 cm dark brown plaque and consisted of an ill-defined, irregular elevation of the skin (Figure 1).
There were no nodules or ulcerations on it. Adjacent lymph nodes were not palpable. A clinical diagnosis of SK was made by dermatologists then after the patient agree, a completely excision was performed.
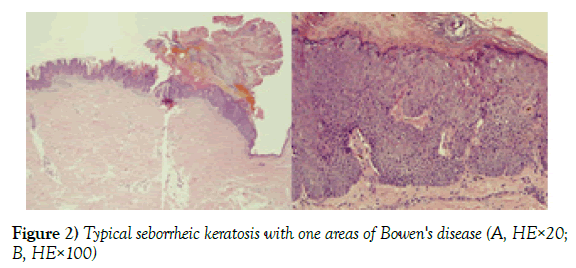
Histologically (Figure 2), the magnification of SK with characteristic acanthosis, papillomatosis and pseudo-horn cysts were present in part of the lesion.
Figure 2) Typical seborrheic keratosis with one areas of Bowen's disease (A, HE×20; B, HE×100)
In another part, atypia of keratinocytes (hyperchromatic nuclei, crowded cells, prominent nucleoli, occasional mitotic figures, several clumping cells, and several individual keratinization) and abnormal mitoses were noted. These changes are full-thickness but no invasion was recognized. There were gradual merges between the two parts. A pathologic diagnosis of BD arising in SK was made.
Discussion
SK was considered as a benign lesion ever since it had been first distinguished with solar keratosis by Freudenthal in 1926 [6]. However, numerous reports and studies showing the possibility of SK malignant transformation have raised questions about the true nature of these so called ‘benign’ lesions [3,7,8]. Common malignant neoplasm in connection with SK were BD, BCC, SCC, keratoacanthoma or even melanoma had been found [9,10]. From a retrospective study of 85,000 clinically diagnosed SK histologic specimens, BCC was the most malignant type with total of 43 lesions, meanwhile 6 specimens contain Bowen disease [8]. However, Vun studied 1813 histologic specimens with the clinically diagnosed as SK, and found BD was the most common non-melanoma skin cancer, in which 36 were BD and 5 were BCCs, and 2 were invasive SCCs [11]. Parvin Rajabi studied 429 SK cases that revealed similar results, they found that 6 lesions associated with malignant transformation among which five cases showed bowenoid transformation [12]. Daniel C Gaffney studied a total of 1987 SK in a high solar UV levels region and indicating that BD was the most frequently observed neoplasm with the rate of 7 percent [4]. These significant difference results are still no conclusions. BD is defined as a intraepidermal carcinoma [13]. SK transformation into BD was first report in 1953 [4]. In the early year studies on this subject, Rowe considered that this phenomenon did not truly represent malignant transformation, and he used the “pseudoepitheliomatous hyperplasia” to designate it [14]. Collision tumour were used to describe SK in association with other lesions either in these years [15]. But debate as whether SK associated with skin cancers represent ‘collision tumours’ or malignant transformation continues. Monteagudo claimed that it is more than pure coincidence as the malignant lesions were not merely adjacent or merging with SK, but were found within SK [11].
In our case, there is a clear transition from typical areas of SK to other regions which are quite compatible with BD, thus satisfying the criteria of malignant transformation. What’s more, it was thought that Bowenoid change within an acanthotic or hyperkeratotic lesion usually located in sunexposed skin [15,16]. Our case is unusual in that it is an example of malignant transformation situated on the back. To conclude, though rare, malignant transformation in what generally considered to be benign lesions SK can happen, and may occur in the absence of sun expose. Surgical removal and a biopsy is required in the clinical diagnosis. And resection should be complete when areas of BD are detected.
Acknowledgements
We thank the patient for granting permission to publish this information. We appreciated the work of surgical and pathological teams involved in the case. This study was supported by National Natural Science Foundation of China (81573063), National Natural Science Foundation of Shanghai (16ZR1431300), Shanghai Municipal Commission of Health and Family Planning (20154Y0196, 20134381). The funders had no role in study design, data analysis, decision to publish, or preparation of the manuscript.
Conflict of Interest
This study does not present any conflicts of interest for us.
REFERENCES
- Hafner C, Vogt T. Seborrheic keratosis. J Dtsch Dermatol Ges 2008;6: 664-77.
- Noiles K, Vender R. Are all seborrheic keratoses benign? Review of the typical lesion and its variants. J Cutan Med Surg 2008;12:203-10.
- Lim C. Seborrhoeic keratoses with associated lesions: a retrospective analysis of 85 lesions. Australas J Dermatol 2006;47:109-13.
- Gaffney DC, Muir JB, De'Ambrosis B. Malignant change in seborrhoeic keratoses in a region with high solar ultraviolet levels. Australas J Dermatol 2014;55:142-4.
- Wu YH, Hsiao PF, Chen CK. Seborrheic keratosis with bowenoid transformation: the immunohistochemical features and its association with human papillomavirus infection. Am J Dermatopathol 2015;37:462-8.
- Monteagudo JC, Jorda E, Terencio C, et al. Squamous cell carcinoma in situ (Bowen's disease) arising in seborrheic keratosis: three lesions in two patients. J Cutan Pathol 1989;16:348-52.
- Bloch PH. Transformation of seborrheic keratosis into Bowen's disease. J Cutan Pathol 1978;5:361-7.
- Cascajo CD, Reichel M, Sánchez JL. Malignant neoplasms associated with seborrheic keratosis. An analysis of 54 cases. Am J Dermatopathol 1996;18:278-82.
- Noiles K, Vender R. Are all seborrheic keratoses benign? Review of the typical lesion and its variants. J Cutan Med Surg 2008; 12: 203-10.
- Madan V, Cox NH, Gangopadhayay M. Porocarcinoma arising in a broad clonal seborrhoeic keratosis. Clin Exp Dermatol 2008; 33: 350-1.
- Vun Y, De'Ambrosis B, Spelman L, et al. Seborrhoeic keratosis and malignancy: collision tumour or malignant transformation. Australas J Dermatol 2006; 47: 106-8.
- Rajabi P, Adibi N, Nematollahi P, et al. Bowenoid transformation in seborrheic keratosis: A retrospective analysis of 429 patients. J Res Med Sci 2012;17:217-21.
- Terada T. Pigmented Bowen disease arising in pigmented reticulated seborrheic keratosis. Int J Clin Oncol 2010;15:608-10.
- Rowe L. Seborrheic keratosis or Pseudo-epitheliomatous hyperplasmia (Weidman). J Invest Dermatol 1957;29:165-80.
- Rigopoulos D, Rallis E, Toumbis-Ioannou E, et al. Seborrhoeic keratosis or occult malignant neoplasm of the skin? J Eur Acad Dermatol Venereol 2002;16:168-70.
- Maize JC, Snider RL. Nonmelanoma skin cancers in association with seborrheic keratoses. Clinicopathologic correlations. Dermatol Surg 1995;21:960-2.