Application of midcab by means of inferior mini sternotomy
2 Coronary Surgery Unit, Cardiac Surgery Center, Tashkent, Uzbekistan, Email: Amansurov@gmail.com
Received: 04-Aug-2017 Accepted Date: Sep 10, 2017; Published: 15-Sep-2017
Citation: Fazliddin S, Abrol M, Ulugbek A, et al. Application of midcab by means of inferior mini sternotomy. Clin Cardiol J 2017;1(1):5-7.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
BACKGROUND: Minimally invasive surgical approach for OPCABG in terms of by using inferior limited mini-sternotomy could benefit for patients in selected category. METHODS: Up-to-date we have operated 18 patients on this technique. Most of the patients were in advanced age and other co morbidities. All patients underwent OPCABG procedure by using inferior sternotomy. In all cases we performed by starting with 5 cm skin incision and sternum opening up to 2nd intercostal space where it could be turned to the left, right or both sides like L- and T-versions. By this way, one can harvest both mammary arteries to revascularize anterior, lateral and posterior walls. The distal anastomosis varied up to 3 depending on target anatomy RESULTS: No in hospital mortality was observed. Conversion to CPB with a full median sternotomy was never required and the anastomosis was carried out through OPCAB mode. The mechanical ventilation time was 3–7 hours. The ICU stay was 13–43 hours. All patients were discharged at 4-6 days after surgery and not observed any complications. CONCLUSION: Limited sternotomy allows to perform single, double and triple vessel revascularization safely off-pump even in high-risk patients
Keywords
Coronary; Artery; Disease; Heart; Ventricular; Cardiomyopathy
Abbreviations
OPCAB: Off Pump Coronary Artery Bypass; CPB: Cardiopulmonary Bypass; ICU: Intensive Care Unit; MIDCAB: Minimally Invasive Direct Coronary Artery Bypass; AMI: Acute Myocardial Infarction; COPD: Chronic Obstructive Pulmonary Disease; LVEF: Left Ventricular Ejection Fraction; AF: Atrial Fibrillation; CCS: Canadian Class System; PCI: Percutaneous Interventions; EDV: End Diastolic Volume; ESV: End Systolic Volume; EDD: End Diastolic Diameter; ESD: End Systolic Diameter; PO: Post-Operative; LIMA: Left Internal Thoracic Artery; RIMA: Right Internal Thoracic Artery; LAD: Left Anterior Descending; RCA: Right Coronary Artery; IMA: Internal Thoracic Artery; TECAB: Total Endoscopic Coronary Artery Bypass
Recent years, we have been facing more coronary patients in older age with high risk severely concomitant diseases. The application of conventional revascularization methods for such patients might lead to negative outcomes with high post-operative complications. Therefore, there have been developed off pump mode coronary artery bypass surgery, minimally invasive coronary bypass surgery (MIDCAB), as well as, the combination of those interventions with interventional methods, named as hybrid procedures [1-8]. These types of surgical treatments are performed in 10-20% of all surgical procedures on ischemic heart disease in leading hospitals of the world [1,3]. Fast recovery, quick wound healing period and short time of hospital discharges give us much favorable impressments of such procedures. On a basis of MIDCAB – the performing of such types of operations on a beating heart without application of heart-lung machine and the using of minimal incisions as a surgical approach. These surgical operations are indicated for old, obese and severely sick patients whom the application of cardiopulmonary bypass might bring worse complications of parenchymal inner organs [1-6].
Methods
We present our single center small cohort of patients in whom it has been performed minimally invasive coronary bypass surgery through inferior mini sternotomy. All 18 consecutive patients: 13 male and 5 female are included in the study, and in all were performed MIDCAB procedure through inferior sternotomy. Here below, you can follow this list of parameters demonstrating our patient’s characteristics (Table 1).
| Male | 13 (72.2) |
| Female | 5 (27.8) |
| Elective operation | 18 (100) |
| Previous AMI | (66.6) |
| Main stem disease | 5 (27.8) |
| COPD | (38.8) |
| Peripheral artery disease | 4 (22.2) |
| Diabetes | 10 (55.5) |
| Hypertension | 16 (88.8) |
| Dislipidemia | 9 (50) |
| Obesity | 8 (44.4) |
| EF <35% | 2 (11.11) |
| EF 35–55% | 10 (55.55) |
| EF >55% | 6 (33.33) |
| Preoperative AF | 3 (16.6) |
| CCS IV | 5 (27.8) |
| CCS III | (72.2) |
| Previous PTCA"Stent | 3(16.6) |
| 1 vessel disease | 12(66.66) |
| 2 vessel disease | 4 (22.22) |
| 3 vessel disease | 2 (11.11) |
| EuroSCORE | average 2.3 |
Table 1: Preoperative characteristics of the population N - 18 Variables No. of patients – (%)
All patients were registered at Coronary Surgery Unit at Republican Specialized Center of Surgery in Uzbekistan. The Data was collected from retrospective analyses of reports at last 1.5 years. All patients presented CCS ¾ classes with concomitant disease as COPD, peripheral artery disease, hypertension, obesity, diabetes and so on. ECHO shows mostly moderate and good EF except severely depressed LVEF in 2 pts. All patients presented quite normal heart volume and size parameters (EDV, ESV, SV, EDD, ESD). The numbers of bypass grafts were performed depending on the number of the coronary lesions and the match consisted of coronary lesions: singe/ double/triple - corresponding to number of patients: 12/4/2, accordingly. In all cases, LIMA-LAD anastomosis were performed firstly and whereas additional grafts necessitated, radial or vein grafts were connected to LIMA in order to complete double or triple bypass surgery. In triple distal anastomosis, the sequential anastomosis was performed on its sequence. All patients were selected into elective case category.
Technical details
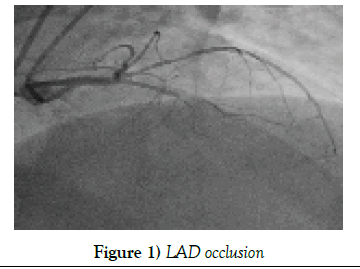
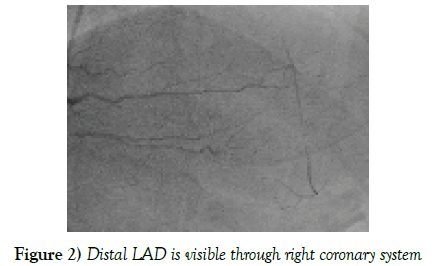
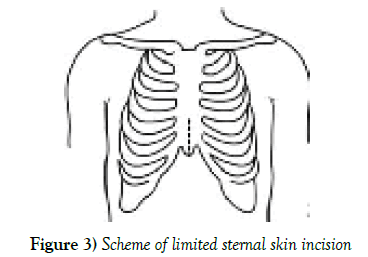
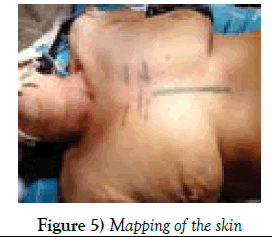
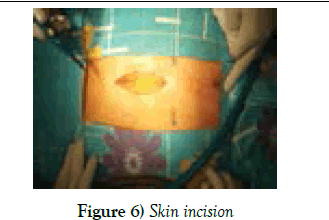
After patient’s intubation and careful mapping for approach is done, up to 5 mm skin incision will be performed on midline sternum (Figures 1-3).
Subcutaneous tissue layer will be spread till the level of 3-4 intercostals. Midline is clearly defined and exposed the left edge of 3-d intercostals space on which line the sternal saw should be gone (Figures 4-6).
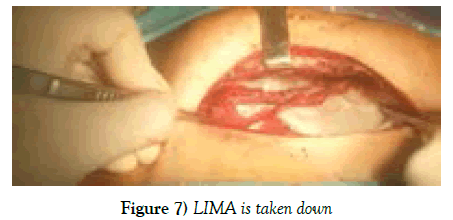
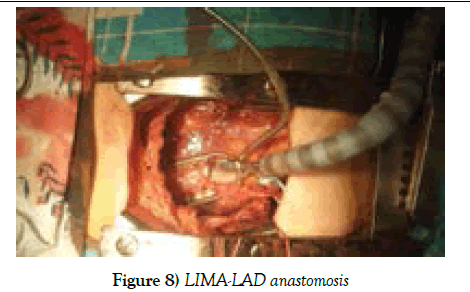
Here, one must to be very careful and think about possible damage of internal thoracic vessels. Inferior partially sternotomy up to 3-d intercostals and sternal retractor setting are described in scheme. The curve edge of the sternum turned to left, right or both sides depending on which IMA is planning to be taken down. During IMA harvest, sometimes, instead of sternal retractor, we have let our assistant to lift the sternal part with Farabeuf hook, as long as the surgeon is harvesting pedicle LIMA, it will take not so long time. And we do not often pay an attention on dissection of 1st intercostal branch, as far as, we studied and learned several studies and finally did not find any true statement of development of “Steal syndrome”. LIMA is dissected distally after injection of 3 mg/kg Heparin (full dose) and wrapped it with Papaverine solution. Pericardiotomy should be made as window-shaped, and left sided pericardial flaps are fixed to the edge of retractor. This manipulation and Trendelenburg position allow the surgeon to make adequate exposure of the anterior surface of the heart. With this approach one can access for diagonal and right coronary system, as well. In order to make anastomosis dry, we applied metal bulldog placement in proximal LAD and take it off after setting of intracoronary shunts. Anastomosis are performed with 8/0 or 7/0 prolene by means of myocardial stabilization (Figures 7-9)
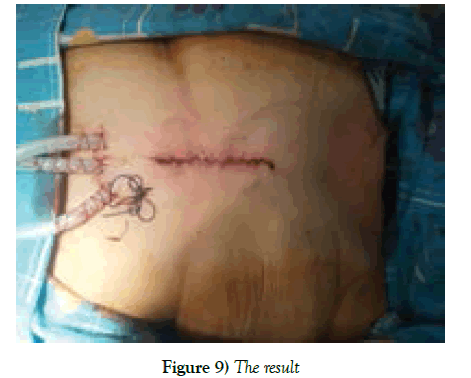
After meticulous hemostasis, drainage tubes and 2 myocardial electrodes are left. Patients are mostly extubated in early hours after operation and transferred to the ward.
Results
During a follow-up period no in-hospital mortality was occurred. No significant changes have been presented towards the volume parameters of the heart. The average ventilation time was 3-7 hours, and ICU stay period was 13-43 hours, consequently. No re-exploration for bleeding has been also occurred. Drainage output in 1 patient was suspicious and the medical management in this case was successful. In first PO day medium drainage output consisted of 220 ± 48.56 ml. All patients were adequate to communicate and present normal neurological functions. A medium PO stay of patients was 4-6 days and all discharged from hospital quite well [5-8].
Discussion
In current era, there are several methods of MIDCAB procedure in treatment of coronary artery disease. Depending on the localization of coronary lesions, MIDCAB might be performed through several approaches as via partially sternotomy, thoracotomy, port-access devices or robotic and endoscopic technologies. We have only started our guide to MIDCAB procedures, and it requires more experienced and equipment facilities. In our series, we completely included patients after inferior partial sternotomy, and via this approach we could do up to 3 bypass grafts as well. If coronary patients describe several concomitant diseases as COPD, diabetes mellitus, chronic heart and kidney failure, they might get easier recovery after MIDCAB in postoperative period [1-3]. Our group of patients there are also presented concomitant diseases mostly hypertensive (16 pt.), COPD (7 pt.), diabetes (10 pt.) and obesity (8 pt.). In such patients, the depending on the constitution of the patients, the harvesting of the internal thoracic arteries are quite difficult. But the overall result of the procedure is nice. The surgical access often depends on the number of coronary lesions and their location in the heart. One vessel disease embraces mostly LAD area is very convenient to perform [1,2]. In our series, 12 patients presented single vessel disease. In which LIMA-LAD was performed. While doing inferior partially sternotomy or lateral thoracotomy, LIMA is easily harvested that might be sufficient to anterior and lateral walls of the heart. We preferred the access through inferior sternotomy, as presented in our series; this approach allows several advantages with limited drawbacks.
Lemma in 2005 presented his series of MIDCAB and prescribed the possibilities of doing anastomosis in several lesions through this approaches. As bypass grafts there are mostly harvested LIMA in order to supply LAD system which occurred in 12 of our patients. Once we required other arteries to be bypassed, we applied radial and vein grafts which are connected to LIMA as Y-shaped grafts, moreover, in situ RIMA graft to bypass RCA system via T-shaped inferior sternotomy was also accomplished. In 4 patients, we have performed double distal anastomosis, where in all 4, the vein grafts were easily connected to LIMA. In 2 patients whom necessitated full arterial grafts, we performed T-shaped sternotomy in order to harvest of both IMA. By the way, this facilitates IMA harvesting from both sides and there was additionally required radial artery to connect to LIMA [9-11].
Inferior sternotomy is easily converted to complete sternotomy and connect the patient to CPB if emergency situation is necessitated. With interior sternotomy, the patients keep their sternum manubrium firmly, by following, no need for breast bandage holding. Moreover, this access provides us such advantages as quick wound recovery, absence of brachial traction injuries, improvement of cosmetic results, early extubation and less being in intensive care unit. Our experience there has been observed 3-7 hours for ventilation time, 13-43 hours for ICU stay and 5-6 days for PO time to discharge. Mini invasive methods for coronary artery diseases permit patients to shorten stationary being for 5-10 days and there needs less recovery period by comparison of conventional methods. Additionally, inflammation related CPB complications, followed after MIDCAB makes circulating blood to face fewer traumas, and CPB adverse effects obviously are reduced. And the patients in a short period after operation return to their normal quality of life. Of course, by development of such techniques, sufficient surgical experience and medical equipment facilities are going to be required in order to get satisfactory outcomes.
MIDCAB by means of hybrid methods, explains MIDCAB combined with PCI procedure helps severely sick patients to be relieved from the symptoms. Although, the literature shows excellent outcomes of complete revascularization after application of hybrid methods, we are under development of this practice. S. Srivastava in 2010 published more than 200 MIDCAB cases in a closed chest (TECAB) with excellent results. Endoscopic and robotic technologies for MIDACB is considered a capital future of coronary surgery and require more financed medical technology and specialized education in leading world hospitals where such kind of procedures are performed more than 100 operation annually.
Conclusion
By the development of coronary surgery, there are going to be performed several variants of coronary operations in order to improve the quality of life of patients who suffer from ischemic heart disease. Our series are also a step-forward technique in development of coronary surgery in Uzbekistan. Inferior sternotomy decreases risk of sternal wound dehiscence and wound infection, provides less risk of traction injuries to the brachial plexus, improves cosmetic results, earlier extubation, and shorter intensive care and hospital stay. It also allows extension to full sternotomy and avoids a second skin incision in emergency cases in which full access is necessary to establish CPB.
To sum it up, we concluded, that MIDCAB by means of partial inferior sternotomy might be performed in a safe and convenient manner with sufficient achievements of surgical outcomes. In the future, we plan to expand our patients’ category with application of various MIDACB technical accesses and study them in long-term period.
REFERENCES
- Gomes WJ, Rogierio A, et al. ALVES/Ministernotomy in off-pump coronary artery by-pass surgery. Braz J Cardiovasc Surg 2005;20(4):377-38.
- Wei L, Yingze L, William CFC, et al. Application of inverted J-shaped partial sternotomy in intracardiac operations. Asian J Surg 2005;28(3)
- Mauro Del G, Andrea DA, Tommaso A, et al. Minimally invasive coronary artery bypass grafting using the inferior J-shaped ministernotomy in high risk patients. Interact Cardiovasc Thorac Surg 2008;7(3):402–06.
- Niinami H, Takeuchi Y, Ichikawa S, et al. Partial median sternotomy as a minimal access for off-pump coronary artery bypass grafting: feasibility of the lower-end sternal splitting approach. Ann Thorac Surg. 2001;72(3):S1041-S5.
- Lichtenberg A, Klima U, Harringer W, et al. Mini-sternotomy for off-pump coronary artery bypass grafting. Ann Thorac Surg. 2000;69(4):1276-7.
- Grandjean JG, Canosa C, Mariani MA, et al. Reversed-J inferior sternotomy for beating heart coronary surgery. Ann Thorac Surg. 1999;67(5):1505-6.
- Gundry SR, Shattuck OH, Razzouk AJ, et al. Facile minimally invasive cardiac surgery via ministernotomy. Ann Thorac Surg 1998;65:1100–4.
- Luo W, Chang C, Chen S. Ministernotomy versus full sternotomy in congenital heart defects: a prospective randomized study. Ann Thorac Surg 2001;71:473–5.
- Del Rizzo DF, Boyd WD, Novick RJ, et al. Safety and cost-effectiveness of MIDCABG in high-risk CABG patients. Ann Thorac Surg 1998;66:1002–1007.
- Calafiore AM, Teodori G, Di Giammarco G, et al. Minimally invasive coronary artery bypass grafting on a beating heart. Ann Thorac Surg 1997;63:S72–S75.
- Detter C, Reichenspurner H, Boehm DH, et al. Single vessel revascularization with beating heart techniques-mini-thoracotomy or sternotomy? Eur J Cardiothorac Surg 2001;19:464-470.