Bilateral gluteus medius tendinous foramina containing portions of the superior gluteal neurovascular bundle
Addison Reed Wood, Rustin Reeves, Armando Rosales*
Department of Cell Biology and Anatomy, University of North Texas Health Science Center, Fort Worth, Texas, USA.
- *Corresponding Author:
- Dr. Armando Rosales, MD
Department of Cell Biology and Anatomy, 3500 Camp Bowie Blvd, Fort Worth, TX 76107, USA.
Tel: +1 (817) 735-2032
E-mail: Armando.Rosales@unthsc.edu
Date of Received: July 17th, 2012
Date of Accepted: November 26th, 2012
Published Online: April 14th, 2013
© Int J Anat Var (IJAV). 2013; 6: 59–60.
[ft_below_content] =>Keywords
gluteus medius, superior gluteal artery, superior gluteal nerve, gluteal variation, foramina
Introduction
The superior gluteal neurovascular bundle passes between the piriformis muscle and gluteus medius muscle as it moves distally to supply the muscles of the gluteal region. The superior gluteal nerve receives spinal contributions from L4, L5, and S1 while the superior gluteal artery is the terminal branch of the posterior division of the internal iliac artery [1]. Multiple variations of the pathway and origin of this neurovascular bundle have been found in the past [2–6]. None of these previous observations show the bundle passing through tendinous foramina made from the surrounding musculature. This is a previously unreported variation in the superior gluteal neurovascular bundle that has significant clinical relevance.
Case Report
A routine dissection of the gluteal region of a 96-year-old female cadaver revealed bilateral tendinous foramina (BTF) that encircled portions of the right and left superior gluteal artery, nerve, and vein. These unique structures have not been previously described within the gluteus medius muscles.
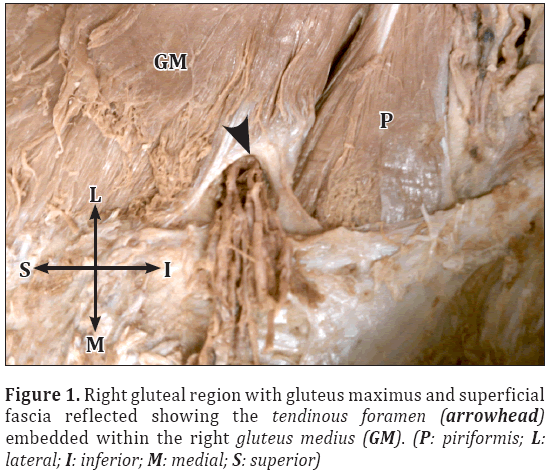
Bilateral tendinous foramina were observed within the inferomedial aspect of the gluteus medius muscles (GMM). The right gluteus medius muscle appeared normal (Figure 1); however, the left gluteus medius muscle had a slight fenestration in its muscle fibers (Figure 2). Near the tendinous foramina, there was a partial separation that divided the left GMM into superolateral and inferomedial muscle segments. Regardless of the minor differences in the right and left GMM, it should be noted that both of these foramina were found within symmetrical locations with respect to the midsagittal plane, and neither pierced any part of the piriformis muscle (Figures 1, 2) [2].
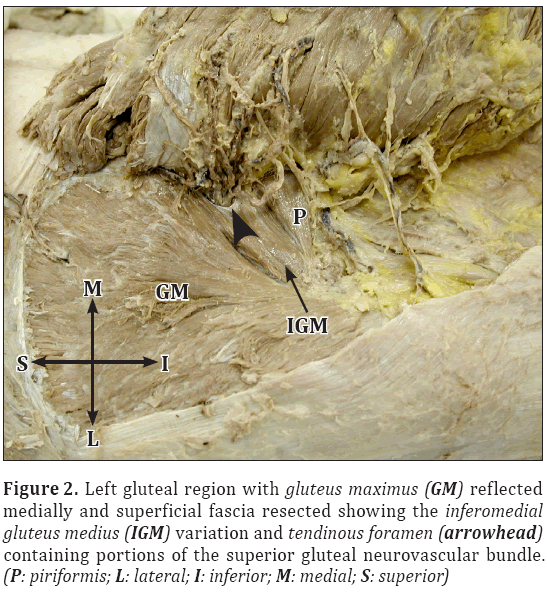
Figure 2: Left gluteal region with gluteus maximus (GM) reflected medially and superficial fascia resected showing the inferomedial gluteus medius (IGM) variation and tendinous foramen (arrowhead) containing portions of the superior gluteal neurovascular bundle. (P: piriformis; L: lateral; I: inferior; M: medial; S: superior)
Approximately two-thirds of the circumference of the foramina were formed by gluteus medius muscle tissue. The medial one-third circumference was formed by the posterosuperior aspect of the greater sciatic foramen and long posterior sacroiliac ligament (Figure 1). These foramina are completely lined on their inner border by what appears as lucid white tendinous tissue. This tissue receives direct contact from the neurovascular bundle and is continuous with the gluteus medius muscle fiber. Superficial branches of the superior gluteal artery and vein passed through the foramina distally in an anterior to posterior (AP) direction. The main trunk of the superior gluteal nerves were not found to pass directly through these foramina in an AP direction; however, smaller branches did follow the superior and inferior deep branches of the superior gluteal arteries and veins (Figure 2) [1]. The superior deep branches of the superior gluteal nerve and vessels initially pass within the inferomedial portion of the gluteus medius muscle near the tendinous foramina. These vessels then run along the superior border of gluteus minimus at its origin between gluteus medius and gluteus minimus [1]. The inferior deep branches of the superior gluteal nerve and vessels were found in the typical position superficial to the gluteus minimus muscle running perpendicular to the axis of the muscle fiber [1].
Discussion
Compression due to anatomical variations in the gluteus medius should be considered by clinicians as a cause of regional gluteal pain and superior gluteal nerve palsy. Hypertrophy of the gluteus medius muscle would increase the likelihood of neurovascular compression with this variation due to the location of the tendinous foramina that contain portions of the superior gluteal neurovascular bundle [2–4]. Clinicians should also be mindful of this rare anatomical variation while performing superior gluteal artery perforator flaps [5], percutaneous iliosacral screw insertion [6], and a multitude of other surgical procedures performed in the same vicinity due to the increased risk of damaging the superior gluteal neurovascular bundle [2–6].
A thorough review of the cadaver’s medical history did not reveal any previous disease or surgical interventions which could serve as a basis for the formation of the bilateral tendinous foramina. Future studies should focus on the frequency of such variations although it would encompass a wide array of variations.
References
- Warwick R, Williams PL, eds. Gray’s Anatomy. 35th Ed., Philadelphia, W. B. Saunders Company. 1973; 567, 671–672, 1055 1057, 1471.
- Smoll NR. Variations of the piriformis and sciatic nerve with clinical consequence: a review. Clin Anat. 2010; 23: 8–17.
- Diop M, Parratte B, Tatu L, Vuillier F, Faure A, Monnier G. Anatomical bases of superior gluteal nerve entrapment syndrome in the suprapiriformis foramen. Surg Radiol Anat. 2002; 24:155–159.
- Rask MR. Superior gluteal nerve entrapment syndrome. Muscle Nerve. 1980; 3: 304–307.
- Kida MY, Takami Y, Ezoe K. The ramification of the superficial branch of the superior gluteal artery. Anatomical basis of a new gluteus maximus myocutaneous flap. Surg Radiol Anat. 1992; 14: 319–323.
- Collinge C, Coons D, Aschenbrenner J. Risks to the superior gluteal neurovascular bundle during percutaneous iliosacral screw insertion: an anatomical cadaver study. J Orthop Trauma. 2005; 19: 96–101.
Addison Reed Wood, Rustin Reeves, Armando Rosales*
Department of Cell Biology and Anatomy, University of North Texas Health Science Center, Fort Worth, Texas, USA.
- *Corresponding Author:
- Dr. Armando Rosales, MD
Department of Cell Biology and Anatomy, 3500 Camp Bowie Blvd, Fort Worth, TX 76107, USA.
Tel: +1 (817) 735-2032
E-mail: Armando.Rosales@unthsc.edu
Date of Received: July 17th, 2012
Date of Accepted: November 26th, 2012
Published Online: April 14th, 2013
© Int J Anat Var (IJAV). 2013; 6: 59–60.
Abstract
Routine dissection of the gluteal region of a female cadaver revealed bilateral tendinous foramina that encircled portions of the right and left superior gluteal artery, nerve, and vein. These unique structures have not been previously described within the gluteus medius muscles. Clinicians should be mindful of this rare anatomical variation while performing surgical procedures in the gluteal region due to the increased risk of damaging the superior gluteal neurovascular bundle.
-Keywords
gluteus medius, superior gluteal artery, superior gluteal nerve, gluteal variation, foramina
Introduction
The superior gluteal neurovascular bundle passes between the piriformis muscle and gluteus medius muscle as it moves distally to supply the muscles of the gluteal region. The superior gluteal nerve receives spinal contributions from L4, L5, and S1 while the superior gluteal artery is the terminal branch of the posterior division of the internal iliac artery [1]. Multiple variations of the pathway and origin of this neurovascular bundle have been found in the past [2–6]. None of these previous observations show the bundle passing through tendinous foramina made from the surrounding musculature. This is a previously unreported variation in the superior gluteal neurovascular bundle that has significant clinical relevance.
Case Report
A routine dissection of the gluteal region of a 96-year-old female cadaver revealed bilateral tendinous foramina (BTF) that encircled portions of the right and left superior gluteal artery, nerve, and vein. These unique structures have not been previously described within the gluteus medius muscles.
Bilateral tendinous foramina were observed within the inferomedial aspect of the gluteus medius muscles (GMM). The right gluteus medius muscle appeared normal (Figure 1); however, the left gluteus medius muscle had a slight fenestration in its muscle fibers (Figure 2). Near the tendinous foramina, there was a partial separation that divided the left GMM into superolateral and inferomedial muscle segments. Regardless of the minor differences in the right and left GMM, it should be noted that both of these foramina were found within symmetrical locations with respect to the midsagittal plane, and neither pierced any part of the piriformis muscle (Figures 1, 2) [2].
Figure 2: Left gluteal region with gluteus maximus (GM) reflected medially and superficial fascia resected showing the inferomedial gluteus medius (IGM) variation and tendinous foramen (arrowhead) containing portions of the superior gluteal neurovascular bundle. (P: piriformis; L: lateral; I: inferior; M: medial; S: superior)
Approximately two-thirds of the circumference of the foramina were formed by gluteus medius muscle tissue. The medial one-third circumference was formed by the posterosuperior aspect of the greater sciatic foramen and long posterior sacroiliac ligament (Figure 1). These foramina are completely lined on their inner border by what appears as lucid white tendinous tissue. This tissue receives direct contact from the neurovascular bundle and is continuous with the gluteus medius muscle fiber. Superficial branches of the superior gluteal artery and vein passed through the foramina distally in an anterior to posterior (AP) direction. The main trunk of the superior gluteal nerves were not found to pass directly through these foramina in an AP direction; however, smaller branches did follow the superior and inferior deep branches of the superior gluteal arteries and veins (Figure 2) [1]. The superior deep branches of the superior gluteal nerve and vessels initially pass within the inferomedial portion of the gluteus medius muscle near the tendinous foramina. These vessels then run along the superior border of gluteus minimus at its origin between gluteus medius and gluteus minimus [1]. The inferior deep branches of the superior gluteal nerve and vessels were found in the typical position superficial to the gluteus minimus muscle running perpendicular to the axis of the muscle fiber [1].
Discussion
Compression due to anatomical variations in the gluteus medius should be considered by clinicians as a cause of regional gluteal pain and superior gluteal nerve palsy. Hypertrophy of the gluteus medius muscle would increase the likelihood of neurovascular compression with this variation due to the location of the tendinous foramina that contain portions of the superior gluteal neurovascular bundle [2–4]. Clinicians should also be mindful of this rare anatomical variation while performing superior gluteal artery perforator flaps [5], percutaneous iliosacral screw insertion [6], and a multitude of other surgical procedures performed in the same vicinity due to the increased risk of damaging the superior gluteal neurovascular bundle [2–6].
A thorough review of the cadaver’s medical history did not reveal any previous disease or surgical interventions which could serve as a basis for the formation of the bilateral tendinous foramina. Future studies should focus on the frequency of such variations although it would encompass a wide array of variations.
References
- Warwick R, Williams PL, eds. Gray’s Anatomy. 35th Ed., Philadelphia, W. B. Saunders Company. 1973; 567, 671–672, 1055 1057, 1471.
- Smoll NR. Variations of the piriformis and sciatic nerve with clinical consequence: a review. Clin Anat. 2010; 23: 8–17.
- Diop M, Parratte B, Tatu L, Vuillier F, Faure A, Monnier G. Anatomical bases of superior gluteal nerve entrapment syndrome in the suprapiriformis foramen. Surg Radiol Anat. 2002; 24:155–159.
- Rask MR. Superior gluteal nerve entrapment syndrome. Muscle Nerve. 1980; 3: 304–307.
- Kida MY, Takami Y, Ezoe K. The ramification of the superficial branch of the superior gluteal artery. Anatomical basis of a new gluteus maximus myocutaneous flap. Surg Radiol Anat. 1992; 14: 319–323.
- Collinge C, Coons D, Aschenbrenner J. Risks to the superior gluteal neurovascular bundle during percutaneous iliosacral screw insertion: an anatomical cadaver study. J Orthop Trauma. 2005; 19: 96–101.