Different WBC count in EDTA caused neutrophil aggregation by hematology analyser
2 Department of medical laboratory science, khomein University of Medical Sciences, Arak, Iran, Email: alireza.mrd39@gmail.com
Received: 16-Mar-2021 Accepted Date: Mar 31, 2021; Published: 07-Apr-2021, DOI: 10.37532/1983-8905.2021.14(3).1-2
Citation: Department of Medical Parasitology and Mycology, Arak University of Medical Sciences, Arak, Iran;2Department of medical laboratory science, khomein University of Medical Sciences, Arak, Iran
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Aggregation of neutrophils in peripheral blood smears is a very rare, mostly self-limiting phenomenon and may result in pseudo leukopenia. The exact reason for neutrophil aggregation in vitro has not been clarified, its relation to the use of ethylene diamine tetra acetate acid as an anticoagulant has been described in adults A 3-year-old boy was referred to Valli e Asr hospital Arak, Iran. The EDTA blood sample was first loaded with the Impedance-based KX-11 Sysmex, which showed a decrease in neutrophils and was observed in the peripheral blood of the Neutrophil aggregation. The blood sample was re-read with the XN-L-350 Sysmex, which is based on the optic method, which showed the number of neutrophils in Norman. Although neutrophil aggregation is extremely rare in daily haematological practice, physicians should be aware of this phenomenon as it may be the cause of leukocytopenia. Therefore, manual differentials should be performed in cases flagged for low leukocyte or neutrophil counts.
Keywords
Neutrophil aggregation, EDTA (Ethylene Diamine Tetra Acetate), Sysmex KX-21, Sysmex XN-L350.Introduction
Due to the wide spread application of automated analyzers for hematological routine tests, spurious results are very likely to occur which should be taken into careful consideration. These out comes might show up as a result of blood cells with serum antibodies interacting as well as reacting with drug or additives in reagents. The effects that repeatedly mentioned are: neutrophil-platelet clumping (satellitism), platelet aggregation and aggregation of nucleated red cells, resulting in pseudo leukocytosis or pseudo thrombocytopenia [1]. A phenomenon less widely spread and more self-constraining in patients who are com of age, is Aggregation of neutrophils in peripheral blood smears, also known as leuko agglutination, neutrophil agglutination, granulocyte aggregation, or leukocyte clumping.
The exact mechanism for neutrophil aggregation in vitro has not been clarified. Its relation to the use of Ethylene Diamine Tetra Acetate acid (EDTA) as an anticoagulant has been described in all reports. Aggregation of neutrophils may result in pseudo leukopenia, thus eliciting further laboratory investigations [2].
Case Presentation
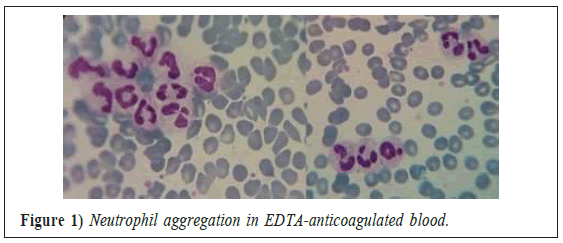
A 3-year-old boy was referred to Valli e Asr hospital Arak, Iran. He was admitted to hospital because of burning in his left arm. He had had no previous illness and was not taking any drugs. A Full Blood Count (FBC) performed on K2EDTA-anticoagulated blood on a Sysmex KX-21 (Sysmex Corporation, Kobe, Japan) showed Red Blood Cell (RBC) count 3.36 ×1012/l, haemoglobin 98 g/l, White Blood Cell (WBC) count 3.2 × 109/l and platelet count 457 × 109/l. A blood film showed neutrophil aggregation (Figure 1). The anticoagulant EDTA is recommended to be 1.4 mg per every blood ml by World Health Organization.
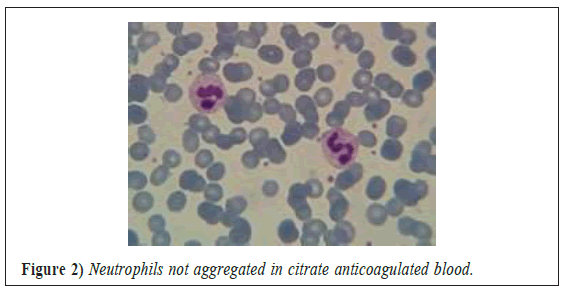
A repeat FBC performed on citrate anticoagulated blood showed a WBC of 10.6 × 109/l. the sodium citrate is recommended 3.2% (109 mmol/L) by WHO [3]. Further investigation of a K2EDTA-anticoagulated sample with a Sysmex XN-L 350, which uses fluorescence flow cytometry, showed a WBC of 10.6 × 109/L (Figure 2).
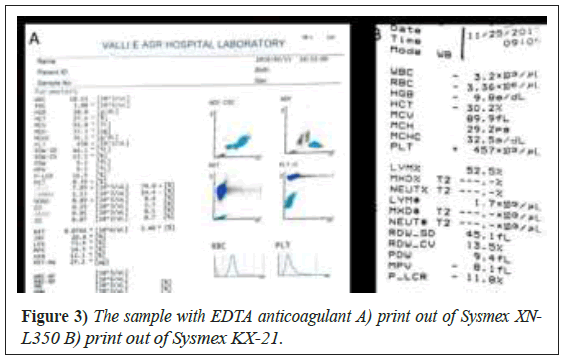
The print out of Sysmex XN-L350 showed no aggregation on sample with EDTA-anticoagulated blood (Figure 3A) but the same sample analysed with the Sysmex KX-21 showed an incorrect WBC (Figure 3A and B).
Results and Discussion
Although the EDTA cause platelet aggregation and satellitism [4], it can neutrophil aggregation [5]. The latter effect has decreased WBC count and change WBC differentiation in automated analyser which use impedance method in counting and shrunken cell size in 3-part differentiation [6]. But this effect is not seen in analyser which uses optic method in counting also in 5 or more-part differentiation on automated analysers use fluorescence staining and optical scatter [7].
Conclusion
In the impedance method the shrunken cell aggregate and cross over the aperture when the antibody put the cell together. But in the analyser which use the optical method due to use of fluorescent dye and sample stream help to separate cell even in the presence of EDTA mediated antibody neutrophil aggregation.
REFERENCES
- Claviez A, Horst HA, Santer R, et al. Neutrophil aggregates in a 13- year-old girl: a rare hematological phenomenon. Ann Hematol. 2003;82(4):251-253.
- Kobayashi S, Seki K, Yamaguchi M, et al. Studies on EDTA-dependent pseudoneutropenia. The Japanese journal of clinical hematology. 1991;32(3):205-211.
- Brittain R. WHO expert committee on biological standardization- WHO. Royal Soc of Health. 1984.
- Weber D, Nakashima M. 198 Platelet Count Stability in Sodium Citrate- Anticoagulated Whole Blood Samples. Am J Clin Pathol. 2018;149:S84- 85.
- Bain BJ. Blood cells: a practical guide: John Wiley & Sons. 2014.
- Gupta A, Gupta P, Bhaghat VM. Interpretation of histograms and its correlation with peripheral smear findings. Platelets. 2017;2(89.4):10-16.
- Tailor H, Mackie I, Mellick A, et al. Evaluation of the Sysmex XN‐550, a Novel Compact Haematology analyser from the XN‐L® series, compared to the XN‐20 system. Int J Lab Hematol. 2017;39(6):585-589.