Future of nurse leadership
Received: 01-Jan-2021 Accepted Date: Jan 15, 2021; Published: 22-Jan-2021
Citation: This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http:// creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Nursing leadership is a crucial part of nurses. Research Moorley have shown that improved leadership in nursing shows improved patient outcomes, increased job satisfaction and lower staff turnover ratio
Keywords
Nursing; Patient; Safety; Leadership; Healthcare
Introduction
In this assignment we are going to discuss patient safety, the application of NMC in nursing practices NMC the national medical commission code is the professional standard that nurses and midwives must maintain to practice in the UK. The NMC is based on four themes; arrange people, perform successfully, reservation of safety and promote competence and trust, and we also discuss the ‘what, so what, now what’ model and how it is applied in nursing leadership. Thus, acquiring clinical leadership skills is crucial for nurses who provide direct patient care. This allows nurses to direct and support patients and healthcare teams when providing care. Furthermore, it is crucial that nurses develop an effective leadership role to deliver high-quality care and ensure patient safety while engaging in numerous daily leadership roles. Moreover, it emphasized the importance of the cooperation between nursing education programs and healthcare organizations in preparing nurses to be effective leaders by 2020 for the new era of health care.
Methods
Task 1
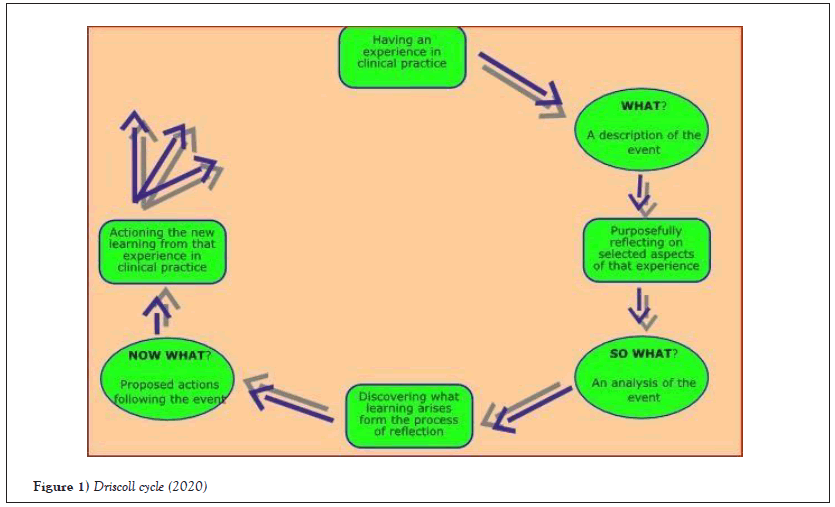
The what? So what? And now what? Driscoll developed a model in the early 1990’s. The model was based on the three questions that were put forward by Terry Borton in the 1970 from these simple questions, we can learn and analyse our experiences from (Figure 1). Firstly, the situation should be described which gives us a clear idea of what are we dealing with. Secondly, the reflective question so what is a result of what have we learned to form the experience [1,2] Figure 1. The third and last stage of the model now what? Talks about the action that we are supposed to take in this reflection, in this stage, we are going to carry something new? The description of the event answers three trigger questions like,
• What is the purpose of returning to the situation and what happed?
• What did I see and do, and what was my reaction to the situation? [3].
So what answers the trigger question such as,
• So what did I feel during the event?
• So what are my feelings now after the situation is it any different from what I had experienced sat that time?
• So what were the effect that I did or did not do, and the purpose of returning to this situation?
Invoking question now what,
• Now, what are the implication for me and others in clinical practice on my studies and what I have described?
• Now, what is the main learning that I can take from reflecting on the practice in this way, and what aspect should be tackled first?
• Now, what shall I do if the same situation arises once again? [4] .
The purpose of going back to the situation was that as there was pressure on the staff with lots of patients in the emergency section and shortage of staff, due to the situation, the nurses present were not able to perform their duties well, I saw patients coming into the ward and most of the cases were due to cold and flu, I tried to help the patient that I attended to while others were waiting, for attending more patients at a time I served two patients at a time, when this confused situation took place a senior nurse suggested that all of us be divided into different departments and communication should be made active so that we could consider each patient quickly, the administration should implement Driscoll model for preventing such cases in the future .
Results and Discussion
Driscoll’s model gives a more in-depth and reflective meaning process by thought provoking enquiry that leads to the formulating of an action plan for the future. I was in the hospital working in the emergency department where many patients were admitted due to influenza, due to a shortage of nursing staff there was much pressure that we faced in this situation [5]. One of our senior staff members divided the prevalent staff to ease the situation and assigned a particular task. By applying the reflection of Driscoll, the implication will help me in enabling to explore several areas for which my experience will improve in the practice of nursing and help me develop the essential skill that will improve the quality of care. The reflection of the Driscoll model will help me in improving my understanding of medical practices. The first skill is to make sure that the communication is improved with the clients for improving the health services in the profession of nursing by understanding the needs of the patients and medical staff for maintaining confidentiality in health practice. I have learned that the level of communication between the nurse and the patient becomes impaired when it is not standardized. Driscoll model will help me in carrying out independent research for establishing the adverse effects of health promotion practices that creates impairment in the process of communication.
Application of Nmc Code
NMC nursing and midwifery council regulates the nursing profession in the UK [6]. The NMC upholds a register of all the nurses in medical health care those who are eligible to practices in the UK. NMC code sets out common standards of behaviour for all those nurses which are registered in the register which gives a clear message to the patients and service users about what can be expected from those who provide nursing and midwifery care.
The code is useful for nurses and for everybody who cares about moral nursing and midwifery.
• Patients can use the NMC code to provide feedback to nurses, and nursing associate about the treatment and care that they receive.
• Nurses who are registered in the NMC code can use it in applying a safe and effective practice in the workplace [7].
• Hospitals should support their staff in following the standards of professional code as a part of giving the quality and safety that are expected by users. The code also contains declarations of what are the practices of nurses and nursing associates.
The code of NMC puts the interest of people by prioritising people, the care of the people is of significant concern and NMC makes sure that their dignity is preserved and the needs of the patients are catered, assessed and responded to. NMC makes sure that those who are receiving care are treated with respect and that their rights are supported [8]. NMC maintains that people are treated with kindness and respect and any discriminatory attitudes are challenged. For treating people as individuals and preserving their dignity the nurse must.
Treat people with kindness, respect and sympathy by making sure that fundamentals of care are effectively delivered
Making sure that any treatment for which the medical staff is responsible is delivered without any delay. For listening to the patient and responding to their preferences and concerns, the code sustains that we must work in partnership for making sure proper and sufficient care is delivered. The basics of care include but are not limited to nourishment, hydration, physical treatment and ensuring that those who are receiving care are appropriately attended. NMC makes sure that those who are receiving care must have easy access to nutrition such as those who are not able to feed themselves or drink any liquid unaided [9].
Standard applied in the hospital
The standards applied in the emergency section of the hospital makes sure that as soon as the patient is admitted, NMC code becomes applicable. Respect the level in which people are receiving care and are involved in the decisions about their health, wellbeing and care. To consider the patients right to be accepted or refused care or treatment. To understand when a patient is anxious or distressed and responding accordingly compassionately and politely [10].
Make sure that people’s physical, social and psychological needs are assessed and responded
For achieving this we must Pay attention to promoting we llbeing and preventing bad health during all the stages of need. Recognise the need for those who are in the last days of their life. Promote any susceptibility and poor practice or any discriminatory attitudes relating to the care of the patient [11].
Performance in the best interests of people at all times
For achieving this, we must make sure that both the nurses and patients are adequately informed before carrying out any professional activity of the practice and all the standards are applied in the particular health care department [12].
Task 2
The relationship between the patient and nurse is of traditional concern in health care research. However, this interaction is examined from a social perspective. There are many problems that the nurse’s face regularly that impacts the performances of nurses some of the problems that the nurses face.
Lack of respect: Most of the nurses feel that there is lack of respect they get from the patients and coworkers as compared to doctors, which makes difficult for nurses to work in an environment where there is no teamwork and respect. It is only possible to work in a team where colleagues respect each other and enjoy working. There have been times where patients become unbearable to nurses to the extent that they become violent [13].
Less compensated: Most of the nurses think that they are not getting paid enough. Nurses want to be compensated more for their job and to get more benefits. Nurses deserve to be well compensated for the hours that they sacrifice.
Insecurity of job: Nurses form a considerable part of the workforce in the health industry. Whenever hospitals/clinics need to cut their cost nurses are first to be targeted. Nurses know that their job is challenging and rewarding and feel that the job does not provide them with a secure future [14].
Working hours are too long: Health care sector involves in a long hour of work, especially nurses, are given in alternative days especially when replacing an absent nurse. Nurses have to have greater strength of mind as well as showing empathy towards their patients, which can be hard to achieve if they have no time to take rest [15].
Multitasking: Like other health care workers, nurses are overloaded with work. When they are stressed, it is hard for them to carry out their responsibilities.
Increased contact with infections: Nurses are more prone to infections as compared to other health care workers, such kind of incidence can occur when an infected patient sneezes or coughs in the middle of a medical procedure. However, using masks and wearing gloves, nurses should also spend money on different supplements so that they are not infected by catching any diseases from the patient to whom they attend [16].
Government involvement: Government of the UK is deeply committed in the sustainability of the long term of the national health services NHS and has put in place to make sure that the system of health care is well placed on preparing for the future. The health department and the national health service in England formed a partnership with the department for communities and the local government association and the association of directors of social services, agree to a medium-term plan that requires for a sustained service transformation at a local level [17].The plan should be covering at least 2025, must be supported by loyal funds and can be implemented by following a full public consultation. In the current legislative framework, considerable progress in the health and social care centre is being made. The “Care Act 2014” amended the national health services Act 2016 by providing better care fund. In addition to the new roles that have been described above, Health education in England leads a programme for embedding a national framework for maximising clinical practice of the nursing and AHP allied health professional workforce [18].
The government has launched a national framework in November 2017. The programme will sanctify in using and developing extended roles for nurses and allied health professional workforce for increasing their nursing skills, knowledge and deployment in the NHS which will be helpful in such cases as staff shortage and an increasing number of patients. The government has also encouraged advanced clinical practice ACP through multi-professional workforce for enhancing the capacity and capability as a part to continue in providing safe, accessible and high quality care for patients [19]. Health education in England and national health services both are working systematically for supporting the expansion of advanced clinical practice that can be capable of a demonstrable impact in high priority areas like accidents and emergency services.
Shortage of nursing refers to a situation where the demand for nursing professionals exceeds supply. It can be measured, when the patient/nurse ratio or nurse/patient ratio necessitates an increased number of nurses that are currently available, shortage in nursing has been observed globally [20]. Nurse staff shortage is not necessarily due to the lack of trained nurses availability. In most cases, shortages occur at the same time with the increased number of students in nursing schools. Factors which include in shortage is lack of proper staff in hospitals and other health care facilities, lack of placement of new nurses, and insufficient worker retaining incentives [21]. The world health organisation had estimated a shortage of almost four million nurses, general physicians and other health care workers were due to underinvestment in health care education, training, fewer salaries, and improper management of the working environment [22]. There are four main reasons behind staff shortage in nursing.
• The growing number of Baby Boomers population, elderly care needs extensive attention.
• Experienced healthcare workforce dropouts.
• Increase in the number of chronic diseases.
• Workload and exhaustion.
Health care institutions have a duty of providing Non-deceptive care to their patients and must make sure that they do not expose patients to unnecessary dangers. If the ratio of nurses and patients are lowered, then such a situation can lead to more complications and poorer outcomes of patients. Once the shortage of staff occurs, the workload for the staff that is remaining will increase, in this event, the patient will not receive expected care [23].
Effects of nursing shortage on patient care: Due to the shortage of nursing staff, nurses have to work for long hours under stressful conditions that results in exhaustion, harm and dissatisfaction in the job. When nurses are exhausted or dissatisfied from the job working in such an environment creates medical errors. Unfortunately, the patient quality can suffer, that can result in a variety of preventable complications, overcrowding in the emergency room and sometimes more severe death cases. Shortage of nurses is the biggest reason of overcrowding in emergency rooms, and it has been reported by [24] that 92% of emergency departments have stated the problem of overcrowding which can cause prolonged hospitalisation, implementation of additional procedures, wrong medical prescription causing permanent disability or death. Overcrowding increases the risk of physicians committing more errors. Shortage of nurses leads to problems like patients waiting for long hours to get to the emergency room [25]. Three out of four hospitals recounted instances where ten patients had to wait for long hours to consult a physician. Improper education and training are one of the common reason for errors in medication while exhaustion and fatigue is the second reason.
The roles and responsibilities of the government are directed basically in achieving national health goals concerning the health of patients, families and communities [26]. In the health sector, government officials provide courses and programmes in leadership and other professional development programmes. Generally, such roles allow nursing in influencing government plans and decisions concerning healthy population and health care provision, one of the most significant things in which the government can invest in public health. Prevention in the early stages is inexpensive which can prevent expensive health care problems later in life. The responsibilities of the government for public health extends beyond voluntary activities, provide services to authorities such as relevant immunisation laws. The partnership of the country functions by encouraging residents to engage in activities that promote their health like physical activity or in creating conditions for promoting good health such as food safety. The areas of public health for which it is accountable are.
• Making sure for adequate public health infrastructure.
• Supporting healthy communities and healthy behaviors.
• Prevention of the spread of communicable disease.
• Protection against environmental dangers concerning health.
• Responding to emergencies and.
• Providing the best health services [27].
The connection between the quality of nursing and patient has been highlighted as a problem in different findings in the NHS national health services, England. Failure in making sure proper nurse staff strength is most commonly cited as a contributing factor in poor health services and staffing of nurses is reported as the primary environmental factor that influences the incidence and occurrence of care that is missed [28]. Evidence supports that the assumption that as low level of nurses that are registered are increasing there are chances that patients are dying on hospital wards due to nonattendance, or delayed care. The involvement of the patient in excellent communication also affects clinical outcomes and safety. Suppose a patient feels that his/her matters are ignored, there are fewer chances that they follow to the advice given to them, if people do not understand what is happening then there are fewer chances for clinical intervention [29].
Conclusion
In conclusion, the care that the patient receives is the direct potential for improvement when the reflective practice of Driscoll model is used it also motivates staff for improving the implementation of professional standards. We have discussed the application of NMC in nursing and health care practices. The problems in nursing concerning shortage of nursing staff in the emergency department with contemporary health care was seen as a problem in health care due to place of work stress that caused higher drop out of nurses in the field of nursing, and we examined how the government is responding to this issue and how those plans are affecting the practice of nursing. A potential cause of a shortage of staff in nursing was due to less payment, overwork, and more turnouts.
REFERENCES
- Moorley C, Chinn T. Developing nursing leadership in social media. J Adv Nurs. 2016;72(3):514-520.
- Cable S, Graham E. “Leading Better Care”: An evaluation of an accelerated coaching intervention for clinical nursing leadership development. J Nurs Manag. 2018;26(5):605-612.
- Roche MR, Duffield CM, Dimitrelis S, et al. Leadership skills for nursing unit managers to decrease intention to leave. 2015.
- Hill B. Exploring the development and identity of advanced practice nursing in the UK. Nurs Manage. 2017;24(5).
- Watson R, McDonagh R, Thompson DR. H-indices: an update on the performance of professors in nursing in the UK. J Adv Nurs. 2016;73(5).
- Francis-Shama J. Perceptions of leadership among final-year undergraduate nursing students. Nurs Manage. 2016;23(7).
- Riva-Mossman S, Kampel T, Cohen C, et al. The Senior Living Lab: an example of nursing leadership. Clin Interv Aging. 2016;11:255.
- McCormack B, McCance T. Person-centred practice in nursing and health care: theory and practice. John Wiley & Sons. 2016.
- Cabral A, Oram C, Allum S. Developing nursing leadership talent—Views from the NHS nursing leadership for south-east England. J Nurs Manag. 2019;27(1):75-83.
- Mingpun R, Srisa-ard B, Jumpamool A. Strengthening preceptors’ competency in Thai clinical nursing. 2015.
- Spilsbury K, Hanratty B, McCaughan D. Supporting nursing in care homes: The RCN Foundation Patient Care and Professional Development for Nursing Staff in Care and Nursing Homes: A Research and Consultation Project. 2015.
- Morris H. Reinstating district nursing: A UK perspective. Nurse Educ Pract. 2017;26:59-63.
- Williams R, Ashton K, Aspinall R, et al. Implementation of the lancet standing commission on liver disease in the UK. Lancet. 2015;386(10008):2098-2111.
- Hafsteinsdóttir TB, van der Zwaag AM, Schuurmans MJ. Leadership mentoring in nursing research, career development and scholarly productivity: A systematic review. Int J Nurs Stud. 2017;75:21-34.
- Carragher J, Gormley K. Leadership and emotional intelligence in nursing and midwifery education and practice: a discussion paper. J Adv Nurs. 2017;73(1):85-96.
- Lin PY, MacLennan S, Hunt N, et al. The influences of nursing transformational leadership style on the quality of nurses’ working lives in Taiwan: a cross-sectional quantitative study. BMC Nurs. 2015;14(1):33.
- Elliott N. Building leadership capacity in advanced nurse practitioners–the role of organisational management. J Nurs Manag. 2017;25(1):77-81.
- Holbery N. Emotional intelligence–essential for trauma nursing. Int Emerg Nurs. 2015;23(1):13-16.
- Recio-Saucedo A, Pope C, Dall'Ora C, et al. Safe staffing for nursing in emergency departments: evidence review. Emerg Med J. 2015;32(11):888-894.
- Kraft M, Kästel A, Eriksson H, et al. Global Nursing—a literature review in the field of education and practice. Nurs Open. 2017;4(3):122-133.
- King R, Tod A, Sanders T. Development and regulation of advanced nurse practitioners in the UK and internationally. Nurs Standard. 2017;32(14):43-50.
- Gorman VLA. Future emergency nursing workforce: what the evidence is telling us. J Emerg Nurs. 2019;45(2):132-136.
- Evans C, Hughes C, Ward K. Improving staff recruitment and retention in the emergency department. Nursing Times. 2017;113(4):18-21.
- Callaghan P, Gamble C. Oxford handbook of mental health nursing. Oxford Handbooks in Nursing. 2015.
- O’Meara P, Wingrove G, Nolan M. Clinical leadership in paramedic services: a narrative synthesis. Int J Health Gov. 2017.
- Bornemann-Shepherd M, Le-Lazar J, Makic MBF, et al. Caring for inpatient boarders in the emergency department: improving safety and patient and staff satisfaction. J Emerg Nurs. 2015;41(1):23-29.
- Donnelly T. Leadership: briefing and debriefing in the operating room. J Perioper Pract. 2017;27(7-8):154-158.
- Brandstorp H, Kirkengen AL, Sterud B, et al. Leadership practice as interaction in primary care emergency team training. Action Res. 2015;13(1):84-101.
- Quinn B. Role of nursing leadership in providing compassionate care. Nurs Standard. 2017;32.