Thrombophilia-related lower limb venous ulceration: A case report
2 Department of Cardiovascular Surgery, Bozok University School of Health, Turkey, Email: meralekim@yahoo.com
Received: 31-Oct-2018 Accepted Date: Dec 03, 2018; Published: 21-Dec-2018
Citation: Ekim M, Kim H. Thrombophilia-related lower limb venous ulceration: A case report. Pulsus J Surg Res. 2018;2(2):76-77
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Venous ulceration is an important disorder affecting about 1% of the adult population and is associated with a significant reduction in quality of life. Post-thrombotic syndrome is a well-known risk factor for leg ulcerations. Approximately 40%-60% of patients with Deep Venous Thrombosis (DVT) suffer from post-thrombotic syndrome; about 10% of them develop venous leg ulceration. Factor V Leiden (FVL) mutation is considered a well-established risk factor for venous thrombosis. Patients with DVT and thrombophilic risk factors have an increased risk of post-thrombotic syndrome because DVT occurs earlier in life and is often recurrent and extensive. More than 40% of patients with chronic venous ulceration have at least one thrombophilic risk factor. FVL mutation was reported to be more frequent in patients with venous leg ulceration than control subjects.
We report a 46-year-old male patient with thrombosed varicose veins and venous skin ulceration around the left internal malleolus. His medical history included DVT about 3 years ago. The heterozygous FVL mutation was detected. His venous leg ulceration improved with a combination of venoactive drug therapy and four-layer compression dressings.
Keywords
Venous ulceration; Thrombophilia; FVL
Introduction
Venous ulceration is an important disorder affecting about 1% of the adult population and is associated with a significant reduction in quality of life [1]. Deep Venous Thrombosis (DVT) is the most common cause of venous leg ulcerations that constitute about 60% of cases [2]. Thrombophilia can be described as an abnormality of the coagulation or fibrinolytic system, which leads to hypercoagulability [3]. It has been reported that hypercoagulable states are associated with the development of lower extremity venous ulceration [4]. Thrombophilia may provide a basis for the development of superficial and deep lower extremity venous reflux as a consequence of macrovascular thromboembolic diseases [5]. Thus, thrombophilia may contribute to the pathogenesis of chronic venous ulceration [5]. Factor V Leiden (FVL) mutation in patients with chronic or recurrent chronic venous ulceration has been suggested to be the most common inherited thrombophilic risk factor [6]. It has been reported that if a patient has venous ulceration in the lower limb and a thromboembolic event occurs before the age of 50 years, the FVL mutation should be investigated [7].
Case Report
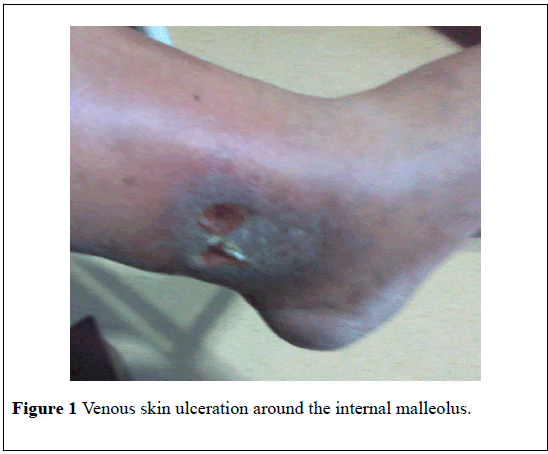
We report a 46-year-old male patient with thrombosed varicose veins and venous skin ulceration around the left internal malleolus. His complaints were swelling, pain and skin ulceration in the left lower extremity. The edges of the ulceration were irregular (Figure 1). The skin surrounding the ulcer was dark colored due to hemosiderin staining. Physical examination findings were normal except venous insufficiency and ulceration findings. The results of liver and kidney function tests were normal. Homocysteine, vitamin B12, and folic acid levels were found to be normal. Venous Doppler examination of the left lower limb revealed venous reflux and thrombosed varicose veins. His medical history included DVT about 3 years ago. The heterozygous FVL mutation was detected. His venous leg ulceration improved with a combination of venoactive drug therapy and four-layer compression dressings.
Discussion
Venous ulceration is one of the most serious complications of Post- Thrombotic Syndrome (PTS) [3]. PTS, a chronic complication of DVT, manifests itself with various symptoms and signs of chronic venous insufficiency. In 5% to 10% of cases, a severe PTS pattern may occur which decreases the quality of life and manifests itself as a venous ulceration [8]. Post-thrombotic syndrome is a well-known risk factor for leg ulcerations. Forty to sixty percent of patients with DVT suffer from post-thrombotic syndrome; about 10% of them develop venous leg ulceration [9]. Patients with DVT and thrombophilic risk factors have an increased risk of post-thrombotic syndrome because DVT occurs earlier in life and is often recurrent and extensive [10].
Venous ulceration is the last stage of the complex of symptoms of chronic venous insufficiency [3]. However, many patients with venous insufficiency will not develop skin ulcers, suggesting that additional factors may play a role in the pathogenesis of venous skin ulcers [4]. It has been suggested that chronic venous ulceration occurs earlier, is more difficult to heal, and relapses more often in patients with hereditary thrombophilic risk factor compared with those without these risk factors [6].
Dahlback et al [11] identified a previously unrecognized mechanism for thromboembolism that is characterized by poor anticoagulant response to Activated Protein C (APC) due to a polymorphism of factor V (FV), in which glutamine replaces arginine, so cleavage of factor V by APC is inhibited [12]. Bertina et al. [13] showed that the phenotype of the APCR is associated with a heterozygous or homozygous single point mutation in the factor V gene (at nucleotide position 1,691, G→A substitution) which predicts the synthesis of a factor V molecule (FV Q506, or FV Leiden) that is not properly inactivated by APC. This mutant FV molecule, called factor V Leiden (FVL), also known as factor V Q506 or Arg506Gln, is named after the city in the Holland where it was first identified [14]. FVL mutation was found to be higher in patients with DVT in Turkish population (41.47%) [15].
More than 40% of patients with chronic venous ulceration have at least one thrombophilic risk factor [16]. FVL mutation was reported to be more frequent in patients with venous leg ulceration than control subjects [3,9]. This mutation is considered a well-established risk factor for venous thrombosis and ulceration [2].
Conclusion
FVL mutation should be investigated in patients with venous ulceration resulting from venous insufficiency associated with DVT. These patients should be monitored closely to prevent DVT recurrences leading to venous ulceration.
Acknowledgements
This study was supported by a grant from Bozok University, The Directorate of Scientific Research Projects (6602c-TF/16-24).
REFERENCES
- Bradbury AW, MacKenzie RK, Burns P, et al. Thrombophilia and chronic venous ulceration. Eur J Vasc Endovasc Surg. 2002;24:97-104.
- McLoone N, Lee B, Anderson J, et al. Homozygous factor V Leiden in a patient with traumatic leg ulceration. Clin Exp Dermatol 2003;28:608-9.
- Darvall KAL, Sam RC, Adam DJ, et al. Higher prevalence of thrombophilia in patients with varicose veins and venous ulcers than controls. J Vasc Surg 2009;49:1235-41.
- Ribeaudeau F, Senet P, Cayuela JM, et al. A prospective coagulation study including resistance to activated protein C and mutations in factors V and ІІ in venous leg ulcers. Br J Dermatol 1999;141:259-63.
- Zutt M, Kruger U, Rosenberger A, et al. Thrombophilia in patients with chronic venous leg ulcers-a study on patients with or without post-thrombotic syndrome. J Eur Acad Dermatol Venereol 2011;25:1432-39.
- Wiszniewski A, Bykowska K, Bilski R, et al. Prevalence rate for inherited thrombophilia in patients with chronic and recurrent venous leg ulceration. Wound Rep Reg 2011;19:552-58.
- Kayatas K, Cebeci F, Karatoprak C, et al. Factor V Leiden mutation-related chronic skin ulcers. Intern J Low extrem wounds 2031;12:35-8.
- Rabinovich A, Kahn SR. The postthrombotic syndrome: current evidence and future challenges. J Thromb Haemost 2017;15:230-41.
- Gaber Y, Siemens HJ, Schmeller W. Resistance to activated protein C due to factor V Leiden mutation: high prevalence in patients with post-thrombotic leg ulcers. Br J Dermatol 2001;144:546-48.
- Katrancıoglu N, Manduz S, Ozen F, et al. Type І plasminogen activator inhibitör 4G allele frequency is associated with venous insufficiency. J Intern Med Res 2010;38:1513-18.
- Dahlback B, Carlsson M, Svensson PJ. Familial thrombophilia due to a previously unrecognized mechanism characterized by poor anticoagulant response to activated protein C: prediction of a cofactor to activated protein C. Proc Natl Acad Sci USA 1993;90:1004-08.
- Kupeli E, Verdi H, Şimsek A, et al. Genetic mutations in Turkish population with pulmonary embolism and deep venous thrombosis. Clin Appl Thromb Hemost 2011;17:E87-E94.
- Bertina RM, Koeleman BP, Koster T, et al. Mutations in blood coagulation factor V associated with resistance to activated protein C. Nature 1994;369:64-7.
- Khan S, Dickerman JD. Hereditary thrombophilia. Thromb J 2006;12:4-15.
- Ekim M, Ekim H. The incidence of FVL and PT G20210A mutations in patients with idiopathic deep venous thrombosis. J Phlebol Lymphol 2018;11:21-4.
- MacKenzie RK, Ludlam CA, Ruckley CV, et al. The prevalence of thrombophilia in patients with chronic venous leg ulceration. J Vasc Surg 2000;35:718-22.