Unusual course of median nerve in arm and forearm
Rajani Singh* and Munish Wadhwan
Department of Anatomy, All India Institute of Medical Sciences, Rishikesh, Uttrakhand 249201 India.
- *Corresponding Author:
- Dr. Rajani Singh
Additional Professor & HOD, Department of anatomy All India Institute of Medical Sci. Virbhadra Marg, Pashulok Rishikesh, Dehradun, UK 249201 India.
Tel: +91 (945) 3193659
E-mail: nani_sahayal@rediffmail.com
Date of Received: November 28th, 2016
Date of Accepted: December 30th, 2016
Published Online: February 3rd, 2017
© Int J Anat Var (IJAV). 2016; 9: 82–84.
[ft_below_content] =>Keywords
median nerve,brachial artery,axillary artery,variation
Introduction
Median nerve is formed by fusion of lateral root from lateral cord and medial root from medial cord in front of axillary artery. In arm it descends down lateral to brachial artery. At the middle of the arm, opposite the insertion of coracobrachialis, the nerve crosses from lateral to the medial side in front of the brachial artery and then the nerve descends medial to the brachial artery and appears in the cubital fossa. In the cubital fossa, the median nerve is medial to the brachial artery. We observed variant configuration of median nerve different from what is described in standard textbooks. Anomalies related to formation, course in hand and the distribution of innervation by median nerve are fairly common. But the variations seen in the present case are quite rare. The variant configuration of median nerve may mislead to confusion in identifying it for repairing damaged median nerve and/or cause complications in other iatrogenic activities. Therefore, Knowledge of these variations is important for surgeons, anesthetists and plastic surgeons for carrying out surgical procedures in the axilla and arm. Hence the case is reported.
Case Report
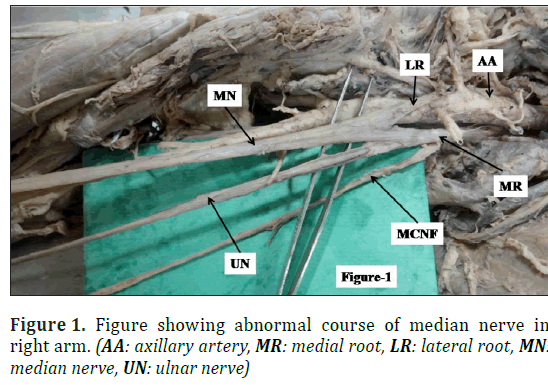
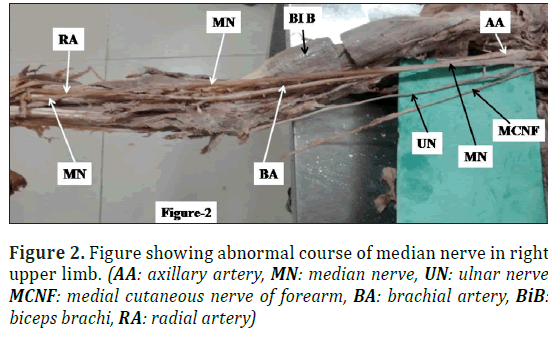
During dissection of right upper limb of female cadaver aged 70 years fixed in 10% formalin in department of Anatomy AIIMS Rishikesh, we observed unusual and variant course of median nerve in arm and fore arm. Median nerve was formed by fusion of lateral root of lateral cord and medial root of medial cord medial to third part of axillary artery (Figure 1). At the junction of upper 1/3rd and lower 2/3rd of arm, median nerve crossed the brachial artery anteriorly from medial to lateral side and in the cubital fossa it remained lateral to brachial artery (Figure 2). Then it descended remaining on the lateral side and at the junction of upper 2/3rd and lower 1/3rd of forearm, it crossed the radial artery from lateral to medial side (Figure 2). There was no unusual observation in the course of median nerve in the hand.
Discussion
Normally median nerve is formed by fusion of two roots; i.e., medial root from medial cord and lateral root from lateral cord lateral to third part of axillary artery and crosses the brachial artery from lateral to medial side. But the variations related to the formation of median nerve by more than two roots are relatively uncommon as compared to the other types of variations of median nerve. In their study, Eglseder and Goldman [1] detected that the median nerve was formed by two lateral roots in 14% of their specimens. Formation of median nerve by fusion of three roots with two lateral roots and one medial root has also been reported [2-4].
There are three well-described entrapment syndromes involving median nerve or its branches, namely carpal tunnel syndrome, pronator teres syndrome and anterior interosseous syndrome. There are few case reports in the literature suggesting the possibility of median nerve entrapment due to a third head of biceps brachii [5,6].
Normally median nerve is formed lateral/anterior to third part of axillary artery, as medial root crosses the axillary artery anteriorly to join with lateral root, lateral to axillary artery. There are reports where median nerve was formed medial to axillary artery [7-9]. They reported median nerve formation medial to third part of axillary artery in 4.7% cases. In these reports the lateral root crossed the axillary artery anteriorly to join with medial root lying medial to axillary artery. Budhiraja et al. [10], in their study on 87 cadavers observed median nerve formation medial to axillary artery in 10.3 % upper limbs. In our case, also median nerve is formed by fusion of two roots medial to third part of axillary artery similar to above reports.
Chitra [7], have reported median nerve to descend medial to brachial artery. Channabasanagouda et al. [11] observed median nerve coursing medial to brachial artery in 3 (6%) of cases.
However, in our case, the median nerve at the junction of upper 1/3rd and lower 2/3rd of arm, crossed the brachial artery anteriorly from medial to lateral side and up to the cubital fossa it remained lateral to brachial artery in contrast to Chitra [7] and Channabasanagouda et al. [11] where the median nerve remained medial to brachial artery. Then it descended remaining laterally and at the junction of upper 2/3rd and lower 1/3rd of forearm, it crossed the radial artery anteriorly from lateral to medial side. Description of such abnormal course of median nerve is rarely available in literature.
The knowledge on the variant pattern of peripheral nerves is essential not only for the surgeons, but also for the radiologists during image and MRI interpretations and for the anesthesiologists before administering anesthetic agents thus in diagnostic approaches [12]. Variations in the course of median nerve are clinically important to avoid injury to it as it may be injured during endoscopic surgery in this region, post traumatic evaluations and peripheral nerve repair. Thus, knowledge of these multiple variations is of immense significance for clinical diagnosis and surgical management of diseases of the upper limb.
Moreover, normal and variant position of the arteries and veins may be determined preoperatively by angiographic studies but in case of nerves it is not possible to detect such an anomaly. Only at the time of surgery the surgeon is exposed to such variations [13]. Descriptions of nerve variations are useful as an anatomical variation can be the cause of a nerve palsy syndrome due to differing relations of a nerve with a related muscle [14]. These are significant sources of misdiagnosis. Thus, knowledge of variant course of median nerve is of paramount importance to surgeons and anatomists.
References
- Eglseder WA Jr, Goldman M. Anatomic variations of the musculocutaneous nerve in the arm.Am J Orthop (Belle Mead NJ). 1997; 26:777–780.
- Chauhan R, Roy TS. Communication between the median and musculocutaneous nerve- a case report. J Anat Soc India. 2002:51:72–75.
- Saeed M, Rufai AA. Median and musculocutaneous nerves: variant formation and distribution. Clin Anat. 2003;16: 453–457.
- George BM, Nayak SM. Median nerve and brachial artery entrapment in the abnormal brachialis muscle- a case report. Neuroanatomy. 2008;7:41-42.
- Mas N, Pelin C, Zagyapan R, Bahar H. Unusual relation of the median nerve with the accessory head of the biceps brachii muscle: an original case report. Int J Morphol. 2006; 24:561–564.
- Paval J. A rare case of possible median nerve entrapment. Neuroanatomy. 2006; 5:35–36.
- Chitra R. Multiple bilateral neuroanatomical variations of the nerves of the arm. Neuroanatomy. 2007; 6: 43-45.
- Singhal, S, Rao VV, Ravindranath R. Variations in brachial plexus and the relationship of median nerve with the axillary artery: a case report. J Brach Plex Periph Nerve Inj. 2007; 2: 21.
- Satyanarayana N, Vishwakarma N, Kumar GP, Guha R, Dattal AK, Sunitha P. Rare variations in the formation of median nerve--embryological basis and clinical significance. Nepal Med Coll J. 2009;11(4):287–290.
- Budhiraja V, R Rastogi, AK Asthana. Variations in the formation of the median nerve and its clinical correlation. FoliaMorphol. 2011; 71(1): 28–30.
- Channabasanagouda, Patil Shrish, Vijaykumar Shinde, P S Jevoor and Madhumati Nidoni. A study of anatomical variations of median nerve in human cadavers. International Journal of Biomedical Research. 2013; 04(12): 682-690.
- Collins JD, ML Shaver, AC Disher and TQ Miller. Compromising abnormalities of the brachial plexus as displayed by magnetic resonance imaging. Clin Anat. 1995; 8(1):1–16.
- Das S, Paul S. Anomalous branching pattern of lateral cord of brachial plexus. Int J Morphol. 2005; 23(4): 289-292.
- Fazan VPS, Amadeu AS, Caleffi AL, Rodrigues Filho OA. Brachial plexus variations in its formation and main branches. Acta Cir Bras. 2003; 18(5): 14-18.
Rajani Singh* and Munish Wadhwan
Department of Anatomy, All India Institute of Medical Sciences, Rishikesh, Uttrakhand 249201 India.
- *Corresponding Author:
- Dr. Rajani Singh
Additional Professor & HOD, Department of anatomy All India Institute of Medical Sci. Virbhadra Marg, Pashulok Rishikesh, Dehradun, UK 249201 India.
Tel: +91 (945) 3193659
E-mail: nani_sahayal@rediffmail.com
Date of Received: November 28th, 2016
Date of Accepted: December 30th, 2016
Published Online: February 3rd, 2017
© Int J Anat Var (IJAV). 2016; 9: 82–84.
Abstract
Median nerve is formed by two roots, one medial root of medial cord and other- lateral root of lateral cord in front/lateral to third part of axillary artery. Then it crosses brachial artery anteriorly from lateral to medial side. In cubital fossa, it remains medial to brachial artery. In forearm, it lays medial to radial artery. We observed unusual formation and course of median nerve during dissection of right upper limb of female cadaver aged 70 years, fixed in 10% formalin in the Department of Anatomy, AIIMS Rishikesh, India. Scanty literature is available describing such variant course of median nerve in arm and forearm. Variations in the course of median nerve are clinically important to avoid injury to it as it may be injured during endoscopic surgery in this region, post traumatic evaluations and peripheral nerve repair. Knowledge of variant course of median nerve is also imperative for radiologists for proper interpretation of radiographs, for anesthesiologists for introducing anesthesia and for anatomists for rare variations.
-Keywords
median nerve,brachial artery,axillary artery,variation
Introduction
Median nerve is formed by fusion of lateral root from lateral cord and medial root from medial cord in front of axillary artery. In arm it descends down lateral to brachial artery. At the middle of the arm, opposite the insertion of coracobrachialis, the nerve crosses from lateral to the medial side in front of the brachial artery and then the nerve descends medial to the brachial artery and appears in the cubital fossa. In the cubital fossa, the median nerve is medial to the brachial artery. We observed variant configuration of median nerve different from what is described in standard textbooks. Anomalies related to formation, course in hand and the distribution of innervation by median nerve are fairly common. But the variations seen in the present case are quite rare. The variant configuration of median nerve may mislead to confusion in identifying it for repairing damaged median nerve and/or cause complications in other iatrogenic activities. Therefore, Knowledge of these variations is important for surgeons, anesthetists and plastic surgeons for carrying out surgical procedures in the axilla and arm. Hence the case is reported.
Case Report
During dissection of right upper limb of female cadaver aged 70 years fixed in 10% formalin in department of Anatomy AIIMS Rishikesh, we observed unusual and variant course of median nerve in arm and fore arm. Median nerve was formed by fusion of lateral root of lateral cord and medial root of medial cord medial to third part of axillary artery (Figure 1). At the junction of upper 1/3rd and lower 2/3rd of arm, median nerve crossed the brachial artery anteriorly from medial to lateral side and in the cubital fossa it remained lateral to brachial artery (Figure 2). Then it descended remaining on the lateral side and at the junction of upper 2/3rd and lower 1/3rd of forearm, it crossed the radial artery from lateral to medial side (Figure 2). There was no unusual observation in the course of median nerve in the hand.
Discussion
Normally median nerve is formed by fusion of two roots; i.e., medial root from medial cord and lateral root from lateral cord lateral to third part of axillary artery and crosses the brachial artery from lateral to medial side. But the variations related to the formation of median nerve by more than two roots are relatively uncommon as compared to the other types of variations of median nerve. In their study, Eglseder and Goldman [1] detected that the median nerve was formed by two lateral roots in 14% of their specimens. Formation of median nerve by fusion of three roots with two lateral roots and one medial root has also been reported [2-4].
There are three well-described entrapment syndromes involving median nerve or its branches, namely carpal tunnel syndrome, pronator teres syndrome and anterior interosseous syndrome. There are few case reports in the literature suggesting the possibility of median nerve entrapment due to a third head of biceps brachii [5,6].
Normally median nerve is formed lateral/anterior to third part of axillary artery, as medial root crosses the axillary artery anteriorly to join with lateral root, lateral to axillary artery. There are reports where median nerve was formed medial to axillary artery [7-9]. They reported median nerve formation medial to third part of axillary artery in 4.7% cases. In these reports the lateral root crossed the axillary artery anteriorly to join with medial root lying medial to axillary artery. Budhiraja et al. [10], in their study on 87 cadavers observed median nerve formation medial to axillary artery in 10.3 % upper limbs. In our case, also median nerve is formed by fusion of two roots medial to third part of axillary artery similar to above reports.
Chitra [7], have reported median nerve to descend medial to brachial artery. Channabasanagouda et al. [11] observed median nerve coursing medial to brachial artery in 3 (6%) of cases.
However, in our case, the median nerve at the junction of upper 1/3rd and lower 2/3rd of arm, crossed the brachial artery anteriorly from medial to lateral side and up to the cubital fossa it remained lateral to brachial artery in contrast to Chitra [7] and Channabasanagouda et al. [11] where the median nerve remained medial to brachial artery. Then it descended remaining laterally and at the junction of upper 2/3rd and lower 1/3rd of forearm, it crossed the radial artery anteriorly from lateral to medial side. Description of such abnormal course of median nerve is rarely available in literature.
The knowledge on the variant pattern of peripheral nerves is essential not only for the surgeons, but also for the radiologists during image and MRI interpretations and for the anesthesiologists before administering anesthetic agents thus in diagnostic approaches [12]. Variations in the course of median nerve are clinically important to avoid injury to it as it may be injured during endoscopic surgery in this region, post traumatic evaluations and peripheral nerve repair. Thus, knowledge of these multiple variations is of immense significance for clinical diagnosis and surgical management of diseases of the upper limb.
Moreover, normal and variant position of the arteries and veins may be determined preoperatively by angiographic studies but in case of nerves it is not possible to detect such an anomaly. Only at the time of surgery the surgeon is exposed to such variations [13]. Descriptions of nerve variations are useful as an anatomical variation can be the cause of a nerve palsy syndrome due to differing relations of a nerve with a related muscle [14]. These are significant sources of misdiagnosis. Thus, knowledge of variant course of median nerve is of paramount importance to surgeons and anatomists.
References
- Eglseder WA Jr, Goldman M. Anatomic variations of the musculocutaneous nerve in the arm.Am J Orthop (Belle Mead NJ). 1997; 26:777–780.
- Chauhan R, Roy TS. Communication between the median and musculocutaneous nerve- a case report. J Anat Soc India. 2002:51:72–75.
- Saeed M, Rufai AA. Median and musculocutaneous nerves: variant formation and distribution. Clin Anat. 2003;16: 453–457.
- George BM, Nayak SM. Median nerve and brachial artery entrapment in the abnormal brachialis muscle- a case report. Neuroanatomy. 2008;7:41-42.
- Mas N, Pelin C, Zagyapan R, Bahar H. Unusual relation of the median nerve with the accessory head of the biceps brachii muscle: an original case report. Int J Morphol. 2006; 24:561–564.
- Paval J. A rare case of possible median nerve entrapment. Neuroanatomy. 2006; 5:35–36.
- Chitra R. Multiple bilateral neuroanatomical variations of the nerves of the arm. Neuroanatomy. 2007; 6: 43-45.
- Singhal, S, Rao VV, Ravindranath R. Variations in brachial plexus and the relationship of median nerve with the axillary artery: a case report. J Brach Plex Periph Nerve Inj. 2007; 2: 21.
- Satyanarayana N, Vishwakarma N, Kumar GP, Guha R, Dattal AK, Sunitha P. Rare variations in the formation of median nerve--embryological basis and clinical significance. Nepal Med Coll J. 2009;11(4):287–290.
- Budhiraja V, R Rastogi, AK Asthana. Variations in the formation of the median nerve and its clinical correlation. FoliaMorphol. 2011; 71(1): 28–30.
- Channabasanagouda, Patil Shrish, Vijaykumar Shinde, P S Jevoor and Madhumati Nidoni. A study of anatomical variations of median nerve in human cadavers. International Journal of Biomedical Research. 2013; 04(12): 682-690.
- Collins JD, ML Shaver, AC Disher and TQ Miller. Compromising abnormalities of the brachial plexus as displayed by magnetic resonance imaging. Clin Anat. 1995; 8(1):1–16.
- Das S, Paul S. Anomalous branching pattern of lateral cord of brachial plexus. Int J Morphol. 2005; 23(4): 289-292.
- Fazan VPS, Amadeu AS, Caleffi AL, Rodrigues Filho OA. Brachial plexus variations in its formation and main branches. Acta Cir Bras. 2003; 18(5): 14-18.