Variant formation and course of the median nerveuniting
Ajay Ratnakarrao Nene*, Krishna Swami Gajendra and Manchiraju Venkata Ramananda Sarma
Department of Anatomy, Ganni Subba Lakshmi Medical College, Andhra Pradesh, India
- *Corresponding Author:
- Ajay Ratnakarrao Nene, MS
Associate Professor, Department of Anatomy, Ganni Subba Lakshmi Medical College, NH-5, Lakshmipuram, Rajahmundry, Dist - East Godavari, Andhra Pradesh, 533296, India
Tel: +91 (883) 2404167
E-mail: ajay.nene@gmail.com
Date of Received: April 21st, 2010
Date of Accepted: June 23rd, 2010
Published Online: July 9th, 2010
IJAV. 2010; 3: 93–94.
[ft_below_content] =>Keywords
median nerve, lateral root, medial root, axillary artery
Introduction
The median nerve (C5, 6, 7, 8; T1) is formed in the axilla by one root each from the medial and lateral cords of brachial plexus. Generally, the medial root derived from the medial cord, (carrying fibers from C8 & T1) joins with the lateral root (carrying fibers from C5, 6 & 7); after crossing the front of the third part of the axillary artery. The median nerve descends anterior to first, the axillary and then, upper part of brachial artery to reach the medial aspect of the brachial artery in the distal half of the arm. It supplies most of the flexor muscles in the anterior aspects of the forearm (C5, 6 & 7) and the thenar and two lumbrical muscles in the hand (C8, T1). It also supplies skin of the hand and fingers but only sympathetic postganglionic fibers to the axillary and brachial arteries in the axilla and arm [1].
Some formative variations of median nerve are documented in the past. The present paper deals with one such formative variation of median nerve, in relation to axillary and brachial arteries.
Case Report
During routine dissection classes of first MBBS students of GSL Medical College, a variant formation of median nerve was observed in the right axilla and arm of a 65-year-old male cadaver. The median nerve was formed by union of two roots, lateral root from lateral cord and medial root from medial cord. But the two roots united posterior to the third part of axillary artery instead of nerveuniting anterior to it. The fork of median nerve thus formed was hooked down by another fork formed by third part of axillary artery and a large common branch giving rise to anterior circumflex humeral, posterior circumflex humeral and profunda brachii arteries. The median nerve thus formed continued posterior to the brachial artery until cubital fossa, where the nerve escaped from the cover of brachial artery and came to lie medial to it. The remaining course and distribution of median was as usual, so was that of brachial artery.
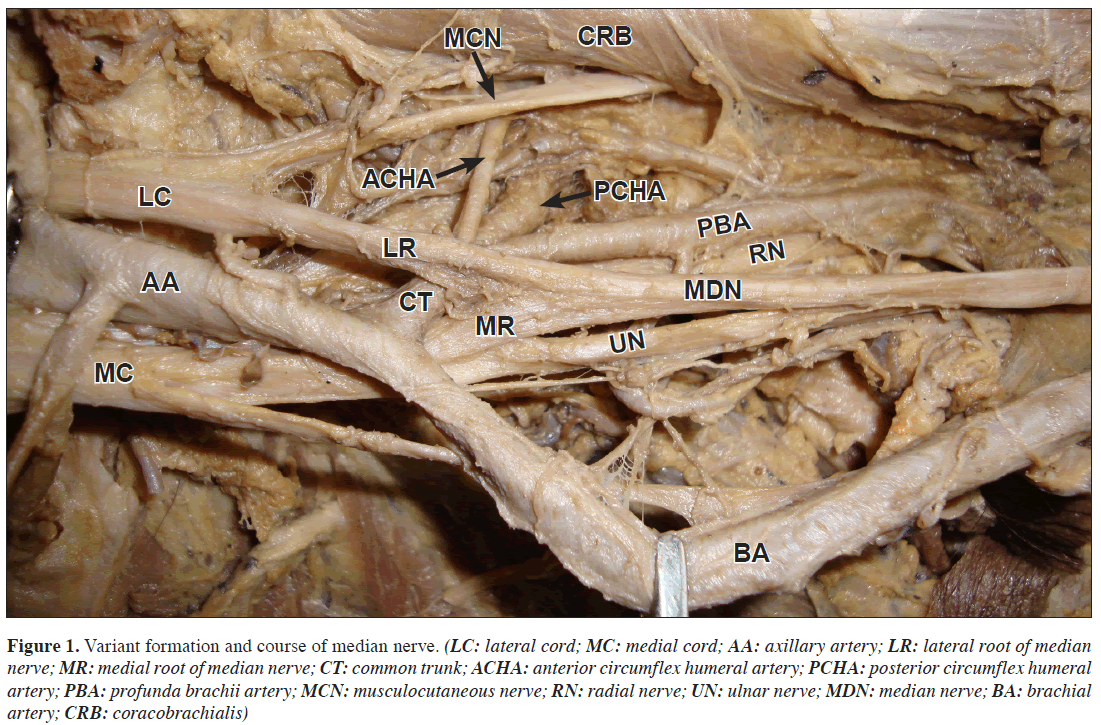
Figure 1: Variant formation and course of median nerve. (LC: lateral cord; MC: medial cord; AA: axillary artery; LR: lateral root of median nerve; MR: medial root of median nerve; CT: common trunk; ACHA: anterior circumflex humeral artery; PCHA: posterior circumflex humeral artery; PBA: profunda brachii artery; MCN: musculocutaneous nerve; RN: radial nerve; UN: ulnar nerve; MDN: median nerve; BA: brachial artery; CRB: coracobrachialis)
Discussion
The formation of the median nerve posterior to the third part of axillary artery is rare and it is not reported in bilateral axillary dissections of 172 cadavers by Pandey and Shukla [2]. In 4.7%, both roots of the median nerve were joined on medial side of the axillary artery to form a median nerve, which traveled medial to the artery in their study. In 2.3%, the roots of the median nerve did not join and both traveled separately anteromedial to the axillary and brachial arteries in the study of the above authors [2].
A somewhat similar picture was reported by Chitra: in one case where the medial root of median nerve would be compressed between axillary and anterior circumflex humeral arteries [3]. Also Haviarova et al. have reported a case in which the formation of median nerve occurred behind the axillary artery on the right side [4]. This type of variation of formation of median nerve and also that of branching of axillary artery are mentioned by Bergman et al. [5,6].
The median nerve may be compressed at its formation in the present case between the axillary artery and the common trunk. Alternatively the third part of axillary artery may be compressed at the site of its branching by the upward fork of formation of median nerve. So, this case report is an example of high median nerve entrapment as well as axillary artery compression. A rare variation of entrapment of the medial root of median nerve between the axillary artery and its variant branch was reported by Vijaya et al. [7]. The knowledge of the high median nerve entrapment is important for the physicians. Also the knowledge of these types of variations is more important in radical neck dissection and in other surgical operation of the axilla.
Conclusion
Variations in formation of median nerve are reported. Knowledge of the variations, especially in relation to a neighboring artery will be of great help to understand the cause and effects of a lesion, both in the nerve and the artery. It will also be helpful to take necessary preoperative precautions and formulate a strategy while planning a surgery in the region.
Embryological explanation for such variations must be sought to understand specific patterns of nerve arrangement and possible associated variations in other nerves and tissues.
References
- Romanes GJ. Cunningham’s Manual of Practical Anatomy. 15th Ed., Volume I, Upper and lower limbs. New York, Oxford University Press. 2003; 70.
- Pandey SK, Shukla VK. Anatomical variations of the cords of brachial plexus and the median nerve. Clin Anat. 2007; 20: 150–156.
- Chitra R. A rare variant formation of the median nerve: a case report. The Internet Journal of Neurology. 2007; Volume 8: Number 2.
- Haviarova Z, el Falougy HA, Killingerova A. Atypical course of the median nerve. Bratisl Lek Listy. 2001; 102: 372–373.
- Bergman R.A, Afifi A.K, Miyauchi R. Illustrated encyclopedia of human anatomic variations: Part III: Nervous system: Plexuses: Median Nerve. http://www.anatomyatlases.org/AnatomicVariants/NervousSystem/Text/MedianNerve.shtml (accessed March 2010)
- Bergman R.A, Afifi A.K, Miyauchi R. Illustrated encyclopedia of human anatomic variations: Opus II: Cardiovascular system: Arteries: Upper limb: Axillary artery. http://www.anatomyatlases.org/AnatomicVariants/Cardiovascular/Text/Arteries/Axillary.shtml (accessed March 2010)
- Vijaya PS, Vollala VR, Mohandas R, Shetty S. A rare entrapment of medial root of median nerve between axillary artery and its anomalous branch. The Internet Journal of Neurology. 2006; Volume 5: Number 2.
Ajay Ratnakarrao Nene*, Krishna Swami Gajendra and Manchiraju Venkata Ramananda Sarma
Department of Anatomy, Ganni Subba Lakshmi Medical College, Andhra Pradesh, India
- *Corresponding Author:
- Ajay Ratnakarrao Nene, MS
Associate Professor, Department of Anatomy, Ganni Subba Lakshmi Medical College, NH-5, Lakshmipuram, Rajahmundry, Dist - East Godavari, Andhra Pradesh, 533296, India
Tel: +91 (883) 2404167
E-mail: ajay.nene@gmail.com
Date of Received: April 21st, 2010
Date of Accepted: June 23rd, 2010
Published Online: July 9th, 2010
IJAV. 2010; 3: 93–94.
Abstract
Many formative variations of median nerve are known but this variant formation and course of median nerve is rare. A variant formation of median nerve was noted in the left axilla and arm of a male cadaver, in the form of formation of median nerve behind the third part of axillary artery and its course in arm entirely behind the brachial artery. There may be compression of axillary artery due to the roots of the nerve passing around the artery. Also there may be compression of median nerve between the fork of axillary artery and its branch. This variation may be clinically important because symptoms of median nerve compression arising from similar variations are often confused with more common causes such as radiculopathy and carpal tunnel syndrome.
-Keywords
median nerve, lateral root, medial root, axillary artery
Introduction
The median nerve (C5, 6, 7, 8; T1) is formed in the axilla by one root each from the medial and lateral cords of brachial plexus. Generally, the medial root derived from the medial cord, (carrying fibers from C8 & T1) joins with the lateral root (carrying fibers from C5, 6 & 7); after crossing the front of the third part of the axillary artery. The median nerve descends anterior to first, the axillary and then, upper part of brachial artery to reach the medial aspect of the brachial artery in the distal half of the arm. It supplies most of the flexor muscles in the anterior aspects of the forearm (C5, 6 & 7) and the thenar and two lumbrical muscles in the hand (C8, T1). It also supplies skin of the hand and fingers but only sympathetic postganglionic fibers to the axillary and brachial arteries in the axilla and arm [1].
Some formative variations of median nerve are documented in the past. The present paper deals with one such formative variation of median nerve, in relation to axillary and brachial arteries.
Case Report
During routine dissection classes of first MBBS students of GSL Medical College, a variant formation of median nerve was observed in the right axilla and arm of a 65-year-old male cadaver. The median nerve was formed by union of two roots, lateral root from lateral cord and medial root from medial cord. But the two roots united posterior to the third part of axillary artery instead of nerveuniting anterior to it. The fork of median nerve thus formed was hooked down by another fork formed by third part of axillary artery and a large common branch giving rise to anterior circumflex humeral, posterior circumflex humeral and profunda brachii arteries. The median nerve thus formed continued posterior to the brachial artery until cubital fossa, where the nerve escaped from the cover of brachial artery and came to lie medial to it. The remaining course and distribution of median was as usual, so was that of brachial artery.
Figure 1: Variant formation and course of median nerve. (LC: lateral cord; MC: medial cord; AA: axillary artery; LR: lateral root of median nerve; MR: medial root of median nerve; CT: common trunk; ACHA: anterior circumflex humeral artery; PCHA: posterior circumflex humeral artery; PBA: profunda brachii artery; MCN: musculocutaneous nerve; RN: radial nerve; UN: ulnar nerve; MDN: median nerve; BA: brachial artery; CRB: coracobrachialis)
Discussion
The formation of the median nerve posterior to the third part of axillary artery is rare and it is not reported in bilateral axillary dissections of 172 cadavers by Pandey and Shukla [2]. In 4.7%, both roots of the median nerve were joined on medial side of the axillary artery to form a median nerve, which traveled medial to the artery in their study. In 2.3%, the roots of the median nerve did not join and both traveled separately anteromedial to the axillary and brachial arteries in the study of the above authors [2].
A somewhat similar picture was reported by Chitra: in one case where the medial root of median nerve would be compressed between axillary and anterior circumflex humeral arteries [3]. Also Haviarova et al. have reported a case in which the formation of median nerve occurred behind the axillary artery on the right side [4]. This type of variation of formation of median nerve and also that of branching of axillary artery are mentioned by Bergman et al. [5,6].
The median nerve may be compressed at its formation in the present case between the axillary artery and the common trunk. Alternatively the third part of axillary artery may be compressed at the site of its branching by the upward fork of formation of median nerve. So, this case report is an example of high median nerve entrapment as well as axillary artery compression. A rare variation of entrapment of the medial root of median nerve between the axillary artery and its variant branch was reported by Vijaya et al. [7]. The knowledge of the high median nerve entrapment is important for the physicians. Also the knowledge of these types of variations is more important in radical neck dissection and in other surgical operation of the axilla.
Conclusion
Variations in formation of median nerve are reported. Knowledge of the variations, especially in relation to a neighboring artery will be of great help to understand the cause and effects of a lesion, both in the nerve and the artery. It will also be helpful to take necessary preoperative precautions and formulate a strategy while planning a surgery in the region.
Embryological explanation for such variations must be sought to understand specific patterns of nerve arrangement and possible associated variations in other nerves and tissues.
References
- Romanes GJ. Cunningham’s Manual of Practical Anatomy. 15th Ed., Volume I, Upper and lower limbs. New York, Oxford University Press. 2003; 70.
- Pandey SK, Shukla VK. Anatomical variations of the cords of brachial plexus and the median nerve. Clin Anat. 2007; 20: 150–156.
- Chitra R. A rare variant formation of the median nerve: a case report. The Internet Journal of Neurology. 2007; Volume 8: Number 2.
- Haviarova Z, el Falougy HA, Killingerova A. Atypical course of the median nerve. Bratisl Lek Listy. 2001; 102: 372–373.
- Bergman R.A, Afifi A.K, Miyauchi R. Illustrated encyclopedia of human anatomic variations: Part III: Nervous system: Plexuses: Median Nerve. http://www.anatomyatlases.org/AnatomicVariants/NervousSystem/Text/MedianNerve.shtml (accessed March 2010)
- Bergman R.A, Afifi A.K, Miyauchi R. Illustrated encyclopedia of human anatomic variations: Opus II: Cardiovascular system: Arteries: Upper limb: Axillary artery. http://www.anatomyatlases.org/AnatomicVariants/Cardiovascular/Text/Arteries/Axillary.shtml (accessed March 2010)
- Vijaya PS, Vollala VR, Mohandas R, Shetty S. A rare entrapment of medial root of median nerve between axillary artery and its anomalous branch. The Internet Journal of Neurology. 2006; Volume 5: Number 2.