Collet-Sicard syndrome: Case report
2 Department of Radiology and Diagnostic by Imaging, Medicine University, Federal University of Goiás, Goiânia, Goiás 74605-050, Brazil, Email: kim.ir.sen@gmail.com
Received: 21-Jan-2019 Accepted Date: Feb 08, 2019; Published: 15-Feb-2019
Citation: Thome de Oliveira IA, Cordeiro BM, Coelho RD, et al. Collet-Sicard syndrome: Case report. J Exp Med Biol. 2019;1(1):16-18.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
Collet-Sicard syndrome is a unique condition involving lesions of the skull base, which affect both the jugular foramen and the hypoglossal canal, affecting the lower cranial nerves IX, X, XI and XII. Symptoms of this pathology include loss of taste in the posterior third of the tongue (IX nerve), vocal cord paralysis and dysphagia (X nerve), weakness in the sternocleidomastoid and trapezius (XI nerve) muscles and atrophy and paresis of the tongue muscles (XII nerve). The present report aims to describe the case in question, referring to a syndrome rare and little described in the literature. In the case of the patient reported, the conduct adopted was to perform radiotherapy sessions in order to prevent tumour progression since the surgery was contraindicated.
Keywords
Collet-Sicard syndrome; Schwannoma; Radiotherapy
Introduction
The first mention of the Collet-Sicard syndrome (CSS) occurred in 1915 by Frederic Collet, in reference to a soldier wounded by bullets during The First World War. Subsequently, Jean A. Sicard made new descriptions, culminating in the name of the syndrome [1].
It is described as a rare condition involving lesions of the base of the skull affecting both the jugular foramen and the hypoglossal canal. It is also known as condylar jugular syndrome, resulting from a unilateral and combined affection of the lower cranial nerves IX, X, XI and XII [2].
The possibilities of cause are numerous (Table 1) and among them it is possible to emphasize: Cranial base metastases, primary intracranial tumours (Example: Schwannoma), extra cranial tumours, trauma, vascular lesions, iatrogenic complications, or inflammatory processes [1].
| Causes of Collet-Sicard Syndrome | No. of cases |
|---|---|
| Skull basemetastasis | 12 |
| Prostate adenocarcinoma | 6 |
| Breast adenocarcinoana | 2 |
| Carcinoma of the uterine cervix | 1 |
| Clear cell renal carcinoma | 1 |
| Disseminated adenocarcinoma | 1 |
| Colon carcinoma | 1 |
| Primary intracranial tumours | 3 |
| Jugular glomus tumour | 2 |
| Neurinoma hypoglossus | 1 |
| Extracranial tumours | 5 |
| Multiple myeloma | 2 |
| Hemangiopericytoma | 2 |
| Neck fibrosarcoma | 1 |
| Trauma | 10 |
| Fracture of skull base | 7 |
| Fracture C l (Jefferson) | 2 |
| Obstric trauma | 1 |
| Vascular | 13 |
| Internal carotid artery dissection | 6 |
| Internal jugular vein thrombosis | 4 |
| Internal carotid artery aneurysm | 2 |
| Internal carotid artery dysplasia | 1 |
| Iatrogeny | 6 |
| Cerebral angiography | 4 |
| Cardiovascular surgery | 1 |
| Cryotherapy of the dental nerve | 1 |
| Inflammatory | 2 |
| Polyarteritis nodosa | 1 |
| Osteomyelitis | 1 |
| Total cases | 51 |
Table 1: Causes of Collet-Sicard Syndrome.
In view of this scenario, the present report aims to describe the case in question, referring to a syndrome rare and little described in the literature, comparing clinical findings with current literature.
Case Report
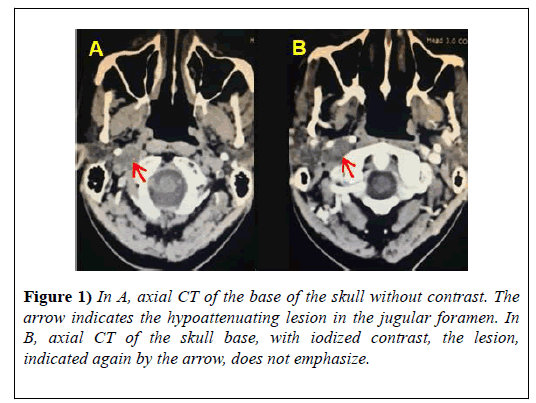
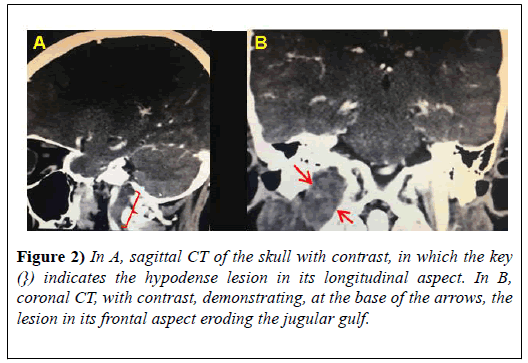
Patient I.L.B, male, 61-years-old, report complaints of dysarthria, dysphagia and reduced tongue mobility. After an otorhinolaryngological evaluation, a CT scan of the skull was requested (Figures 1A and 1B, Figures 2A and 2B) which localized expansive, solid, slow- growing, hypovascular formation located in the jugular foramen and extending inferiorly to the right carotid space of probable neoplastic etiology.
The main hypothesis considered is schwannoma. Subsequent referral to the neurologist and evaluation after detailed neurological examination showed a deviation of the tongue to the right side with right atrophy, difficulty in elevating the shoulder and paresis of the right lateral aspect of the neck. In addition to the reported symptoms, there were no alterations in other pairs of cranial nerves and other systems.
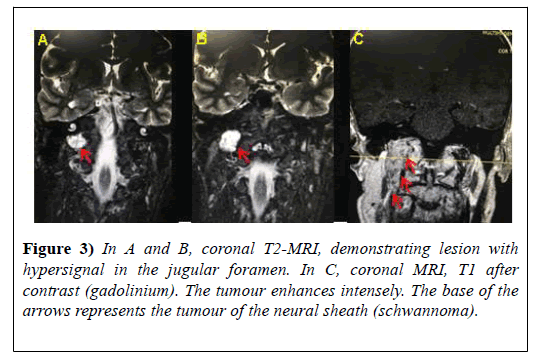
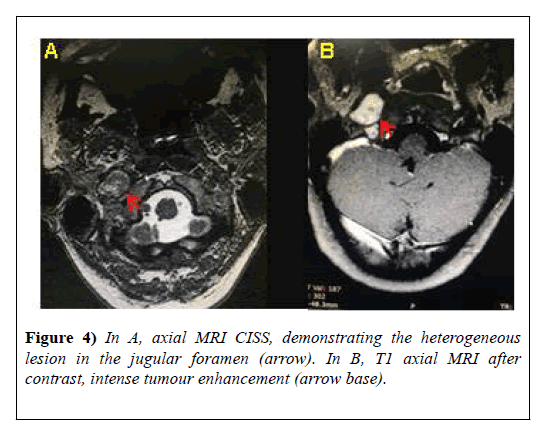
In Magnetic Resonance Imaging (MRI) (Figures 3A-3C, Figures 4A and 4B), the neoplastic etiology for the neural sheath tumour (schwannoma) is confirmed. The next step was to refer the patient to the radiotherapy, after consulting the neurosurgeon who contraindicated surgery because of the presence of risks to damages in important brain areas and irreversible damage to the corresponding cranial nerves, which could lead to a total loss of their functions. Several radiotherapy sessions were performed without satisfactory results.
Discussion
The symptomatology of Collet-Sicard syndrome described in the literature [3] involve loss of taste in the posterior third of the tongue (IX nerve), paralysis of the vocal cords and dysphagias (X nerve), weakness in the sternocleidomastoid and trapezius muscles (XI nerve) and atrophy and paresis of the tongue muscles (nerve XII). Symptoms manifested by I.L.B.
Most intracranial primary tumours affect adults, especially from 45 to 50 years, and among the causes, the most frequent are vascular [4]. The cause of CSS in the patient in question was the intracranial tumour in the neural sheath (schwannoma). Schwannomas are benign tumours, which develop mainly in the sensory part of the nerves (VIII and X) and rarely affect the nerve XII [5]. They mainly affect the female sex, and may be related to hereditary syndromes and exposure to ionizing radiation. By affecting important cranial nerves the surgery is controversial [6]. In this sense, the most recommended treatment is the neuroradiological follow-up associated with curative radiotherapy because it is a slowly evolving tumour. This therapy may be associated with microsurgical resection [7].
In the case of the patient reported, the conduct adopted was the accomplishment of radiotherapy sessions. Surgery was contraindicated due to the risk of affecting the sensitivity and tasting of the posterior third of the tongue, laryngeal and palate sensitivity, speech, sternocleidomastoid and hypoglossal muscle movements and tongue on the injured side if there were intercurrences. However, tongue movement, swallowing and elevation of the right shoulder were affected and there was no improvement after treatment.
Conclusion and Final Considerations
The present approach on Collet-Sicard syndrome is of extreme relevance for the medical community because it is a rare occurrence with few cases reported. In view of this it is important to question whether the reported syndrome is an underdiagnosed disease or whether it constitutes a really rare condition. Therefore, investments in researches and studies in this area are extremely relevant.
The symptoms initially reported by the patient and the adoption of radiotherapeutic therapy converge with data found in the literature in which the radiotherapeutic alternative is predominant. In addition, there is no vast database of the rare syndrome, therefore, studies on comorbidity are still necessary in order to improve the associated symptomatology. Therefore, it is of fundamental importance to continue research on Collet- Sicard syndrome, including its symptoms, diagnosis, treatment and clinical evolution, since it is a rare condition and still little described in the literature.
Acknowledgement
Appreciation to Professor Kim-Ir-Sen Santos Teixeira Radiologist and Head of the Department of Radiology and Diagnostic Imaging of the Faculty of Medicine of the Federal University of Goiás (UFG) and the Diagnostic Imaging Clinic for the support in the manuscript and availability of the iconographies used.
REFERENCES
- Gutiérrez Ríos R, Castrillo Sanz A, Gil Polo C, et al. Collet-Sicard syndrome. Neurologia. 2015;130-2.
- Mnari W, Kilani M, Harrathi K, et al. An unusual etiology of posttraumatic Collet–Sicard Syndrome: A case report. Pan Afr Med J. 2016.143.
- Bravo F, Martorelli SBF, Martorelli FO, et al. The collet-sicard syndrome and dentistry: A case report. RGO- Revista Gaúcha de Odontologia. 2018;177-80.
- Brasileiro Filho G. Bogliolo pathology. (9th edtn). Rio de Janeiro: Guanabara Koogan. 2017.
- Lee SH, Lee ES, Neo CH, et al. Collet-Sicard syndrome with hypoglossal nerve schwannoma: A case report. Ann Rehabil Med. 2017; 1100-04.
- Muzevic D, Legcevic J, Splavski B, et al. Stereotactic radiotherapy for vestibular schwannoma. Cochrane Database Syst Rev. 2014;1-13.
- National Cancer Institute José Alencar Gomes Da Silva (INCA). Brazil. 2018.