Hepatocellular carcinoma and cholangiocarcinoma: A case study report
2 Department of Autopsy Histopathology, Laboratory of Forensic Medicine and Toxicology, Aristotle University of Thessaloniki, Greece, Email: polyanthi@gmail.com
3 Surgical Department, General Hospital “AHEPAâ€, ThessalonIki, Greece
4 Laboratory of Forensic Medicine, Medical School, Democritus University of Thrace, Greece
Received: 03-Apr-2018 Accepted Date: Apr 28, 2018; Published: 10-May-2018
Citation: Dimitriadis I, Konstantinidou P, Givannakis M.I, et al. Hepatocellular Carcinoma and Cholangiocarcinoma: A case study report. J Histol Histopathol Res 2018;2(1): 8-10.
This open-access article is distributed under the terms of the Creative Commons Attribution Non-Commercial License (CC BY-NC) (http://creativecommons.org/licenses/by-nc/4.0/), which permits reuse, distribution and reproduction of the article, provided that the original work is properly cited and the reuse is restricted to noncommercial purposes. For commercial reuse, contact reprints@pulsus.com
Abstract
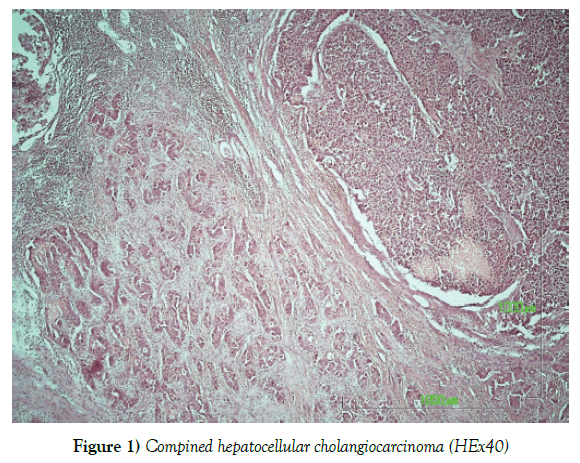
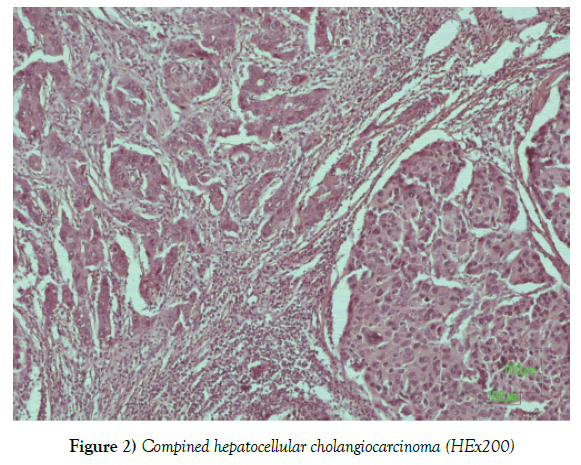
Combined hepatocellular cholangiocarcinoma [HCC-CC] is a rare form of primary liver cancer, showing a mixture of hepatocellular and biliary features. Data suggest that most CHC arise from hepatic progenitor cells [HPCs]. Recent classification of combined HCC-CC is usually based on three categories separate type, transitional type and intermediate type. The case reported below, concerns the incident of a liver tissue measuring 11 × 8.5 × 4 cm. and weighing 155 gr. with an adjacent fatty area of 12 × 6 × 3 cm and an adherent gall bladder, 8.5 cm in length and 5 cm in diameter. We investigated the type of HCC-CC and immunophenotypes using different hepatic progenitor cell markers and classic histological staining technique.
Keywords
Hepatcellular carcinoma, Cholangiocarcinoma,, Liver cancer
Introduction
Combined hepatocellular carcinoma and cholangiocarcinoma is the most common primary liver cancer worldwide. Another primary liver cancer is intrahepatic cholangiocarcinoma. HCC –CC is the sixth most common lethal malignancy for men and the 10th for women in the US, with approximately 300,000-1,000,000 new cases per year, and the incidence is not among the top 10 in both sexes. It is more common in countries like Japan, Africa, South-East Asia, Italy and Greece, compared to North America, Britain and other European countries. The incidence of the disease is steadily rising, while in the United States it has doubled over the past 30 years, and perhaps this increase is related to HCV infection and migration [1,2]. The male / female ratio is 3.7 : 1 except for cases where there is no pre-existing liver disease where the ratio is 1: 1. Recent studies indicate that the disease is present in younger ages [40-60 years], although it is rare in children. Genetic predisposition to different races or ethnic groups has not been demonstrated, and its preference for men is more likely to be related to the greater exposure of men to environmental factors associated with the disease [HBV, HCV, alcoholism, etc.]. In the majority of patients it develops in a background of fibrosis or cirrhosis due to hepatitis B or C or alcoholism, but it can also develop in the absence of this background [3,4]. Recent classification of combined HCC-CC is usually based on three categories: i) separate type in which the tumor consists of varying degrees of a combination of moderately differentiated HCC with a trabecular pattern and CC with a tubular pattern and abundant fibrous stroma, ii) transitional type, in which the CC element with its tubular pattern and fibrous stroma is contiguous with HCC elements having a trabecular or solid pattern, iii) the intermediate type in which HCC elements and CC elements are almost indistinguishable, and the tumors cells are hyperchromatic [5-7].
Materials and Methods
We received a liver tissue measuring 11 × 8.5 × 4 cm. and weighing 155 gr., with an adjacent fatty tissue of 12 × 6 × 3 cm and an adherent gall bladder, 8.5 cm in length and 5 cm in diameter. The tissue sections were stained with Hematoxylin and Eosin [H & E] staining technique. The procedure was:
• Deparaffinize the section: flame the slide on burner and place in the xylene. Repeat the treatment.
• Hydration: Hydrate the tissue section by passing through decreasing concentration of alcohol baths and water. (100%, 90%, 80%, 70%)
• Stain in hematoxylin for 4 minutes.
• Wash in running tap water until sections “blue” for 5 minutes or less.
• Differentiate in 1% acid alcohol (1% HCl in 70% alcohol) for 1 second.
• Wash in running tap water.
• Stain in Eosin for 2 minutes.
• Dehydrate in increasing concentration of alcohols and clear in xylene.
• Mount in mounting media.
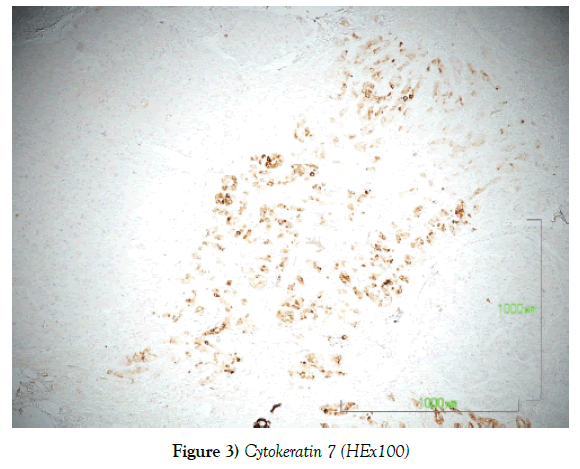
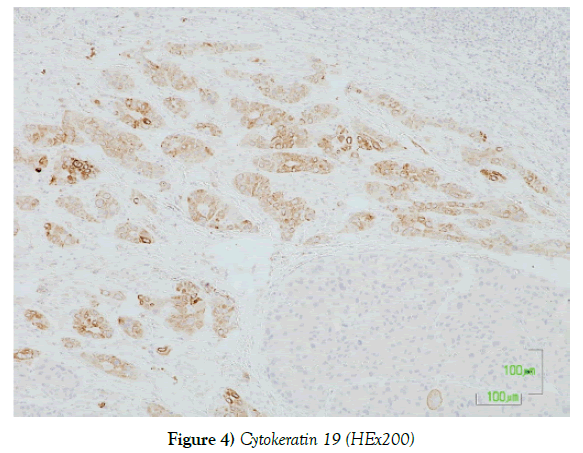
• We also examine the tissue using immunohistochemistry technique with the cell markers AE1/AE3, AFP, Hepar-1, Ck 7 and Ck 19. After the staining procedure the sections observed under microscope and the results conducted.
Results
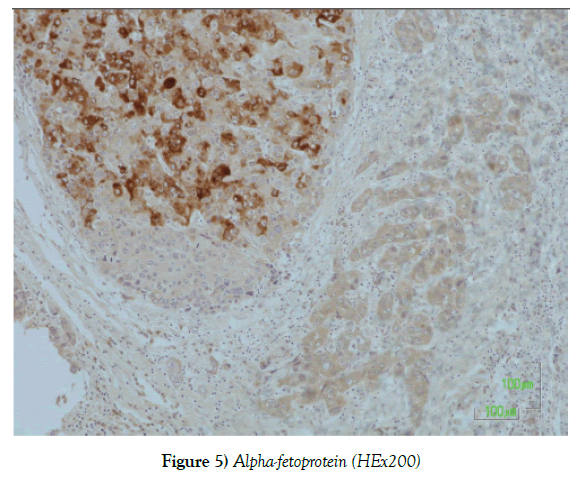
The histological examination of the incisions from the above macroscopically described tumor showed a biphasic presence of malignant neoplastic elements consisting of hepatocellular carcinoma in the form of nodules, with the presence of cholangiocarcinoma areas. The two malignant neoplasms are closely mixed, but their classical morphology remains. The hepatocellular carcinoma element is poorly differentiated and immunohistochemically expresses the markers AE1 / AE3, AFP [focal positivity], Hepar-1 [focal positivity], while the cholangiocarcinoma element shows positivity to the markers Ck 7, Ck 19 and AE1 / AE3 (Figures 1-5).
Discussion
The diagnosis is usually performed in the context of control and monitoring of high-risk patients [cirrhotic, hepatitis, etc.] or randomized control for unrelated reason. The pick of the diagnosis is imaging examinations: ultrasound with or without contrast diluents, CT scan with or without angiography and MRI. Blood tests vary and are not diagnostic of hepatocellular carcinoma but show the patient’s physical condition. Even cancer markers such as Alpha-Phetoprotein have no purely diagnostic role but rather supportive preoperative and control and follow-up postoperatively, since their preoperative values were high. Special reference should be made to the biopsy of the lesion, which should be done in a very limited number of cases to none at all [8,9]. Nowadays, in the majority of cases, the diagnostic imaging tests that are performed enable precise pre-operative diagnosis. There are very few cases where imaging does not provide a clear diagnosis, but even then we have to ask ourselves whether the clear diagnosis that the biopsy can give us will affect our treatment strategy. If there is a liver tumor that will anyway be treated, nothing will help us with a biopsy that involves the risk of bleeding and spreading cancer [10,11]. Conversely, a biopsy not from the damage but from the normal parenchyma may in some cases be needed to assess the quality and condition of the liver parenchyma that will remain after the resection.
Conclusion
The most widespread treatment is surgical resection. Transplantation is indicated in some patients under certain conditions, but given the reduced availability of transplants, this treatment is not as broad as it is not for all those with hepatocellular cancer but only for some who meet the criteria [12]. Other modes of treatment that are always compared to their efficacy with the resection that is the comparison measure are RF ablation, microwave ablation and arterial injection. Surgical resection is a treatment that requires planning to achieve the maximum possible therapeutic effect for a particular tumor in a particular patient.
REFERENCES
- Kojito M. Combined hepatocellular carcinoma and cholaniocarcinoma. In: Kojito M, editor. HCC Blackwell 2006:100-25.
- Kim H, Park C, Han KH, et al. Primary liver carcinoma of intermediate (hepatocyte- cholangiocyte) phenotype. J Hepatol 2004;40(2):298-307.
- Edge SB, Byrd DR, Compton CC, et al. AJCC cancer staging manual. New York: Springer, 2010.
- Cai X, Zhai J, Kaplan DE, et al. Background progenitor activation is associated with recurrence after hepatectomy of combined hepatocellular-cholangiocarcinoma. Hepatol 2012;56(5):1804-16.
- Li L, Qian M, Chen IH, et al. Acquisition of Cholangiocarcinoma Traits during Advanced Hepatocellular Carcinoma Development in Mice. Am J Pathol 2018;188(3):656-71.
- Zhang F, Chen XP, Zhang W, et al. Combined hepatocellular cholangiocarcinoma originating from hepatic progenitor cells: immunohistochemical and double-fluorescence immunostaining evidence. Histopathol 2008;52(2):224-32.
- Kim H, Park YN. Hepatocellular carcinomas expressing 'stemness'-related markers: clinicopathological characteristics. Dig Dis 2014;32(6):778-85.
- Cai X, Xiong J, Hu QG, et al. Look into hepatic progenitor cell associated trait: Histological heterogeneity of hepatitis B-related combined hepatocellular-cholangiocarcinoma. J Huazhong Univ Sci Technolog Med Sci 2017;37(6):873-79.
- Theise ND, Yao JL, Harada K, et al. Hepatic ‘stem cell’ malignancies in adults: four cases. Histopathol 2003;43(3):263-71.
- Libbercht L. Hepatic progenitor cells in human liver tumor development. World J Gastroenterol 2006;12(39):6261-5.
- Yano Y, Yamamoto J, Kosuge T, et al. Combined hepatocellular and cholangiocarcinoma: a clinicopathologic study of 26 resected cases. Jpn J Clin Oncol 2003;33(6):283-7.
- Koh KC, Lee H, Choi MS, et al. Clinicopathologic features and prognosis of combined hepatocellular cholangiocarcinoma. Am J Surg 2005;189(1):120-5.